
Here's the good news: gingivitis is completely reversible when caught early. Unlike advanced periodontal disease, which causes permanent bone loss, gingivitis affects only the soft gum tissue. With the right approach—improved oral hygiene and professional care—you can restore your gums to full health within weeks. This article explains exactly how gingivitis develops, the warning signs to watch for, and the proven steps to reverse it before it progresses to something more serious.
TL;DR
- Plaque bacteria cause gingivitis within hours if not removed, hardening into tartar in 24-48 hours
- Early signs include red, swollen gums that bleed during brushing, persistent bad breath, and gum tenderness
- Reversible through professional cleaning, daily brushing and flossing, and antiseptic mouthwash
- Untreated gingivitis progresses to periodontitis, causing irreversible bone loss and potential tooth loss
What Is Gingivitis?
Gingivitis is inflammation of the gum tissue that bacterial infection triggers. It's the mildest form of periodontal disease—and the most treatable.
The critical distinction between gingivitis and advanced gum disease lies in what's damaged:
- Gingivitis affects only the soft gum tissue — There's no migration of the tissue attachment point and no loss of underlying bone or periodontal ligament, which is why it's reversible
- Periodontitis involves irreversible destruction — Once inflammation extends to supporting structures, causing bone loss and tissue attachment loss, the damage cannot be undone
This reversibility makes early detection crucial. The National Institute of Dental and Craniofacial Research reports that 42% of U.S. adults aged 30+ already have periodontitis. Since gingivitis precedes periodontitis, its prevalence is significantly higher—affecting most adults at some point in their lives.
Common Causes of Gingivitis
Gingivitis typically develops when one or more risk factors allow bacteria to accumulate and infect gum tissue. Understanding these causes helps you identify which factors apply to your situation.
Plaque and Tartar Buildup
Plaque is a sticky, colorless film of bacteria that forms on your teeth shortly after eating starches and sugars. The timeline from plaque to hardened tartar is surprisingly rapid:
| Stage | Timeline | What Happens |
|---|---|---|
| Plaque Formation | Minutes to hours | Bacterial film forms on teeth after eating |
| Mineralization Begins | 24-48 hours | Plaque starts hardening into calculus (tartar) |
| Full Calcification | 12 days | Plaque reaches 60-90% calcification; professional removal required |
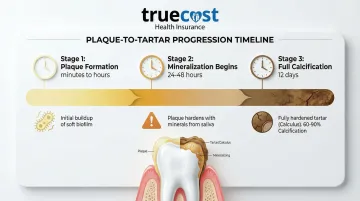
Once plaque mineralizes into tartar, you can't remove it with brushing alone. It requires professional scaling by a dentist or hygienist.
Common causes of tartar buildup:
- Brushing inconsistently or skipping days
- Missing hard-to-reach areas between teeth
- Skipping regular dental cleanings
Poor Oral Hygiene Technique
Even people who brush daily may develop gingivitis if their technique is inadequate. The American Dental Association provides specific guidelines:
- Duration: Brush for 2 minutes—studies show this achieves significantly greater plaque reduction than shorter brushing
- Angle: Position the brush at a 45-degree angle to the gumline
- Motion: Use gentle, short back-and-forth strokes
- Frequency: Brush twice daily with a soft-bristled brush
Brushing too hard, using the wrong angle, or rushing through the process leaves plaque behind, especially along the gumline where gingivitis starts.
Smoking and Tobacco Use
Smoking creates a paradox that makes gingivitis harder to detect. While smokers face nearly twice the risk of gum inflammation, they exhibit approximately 40% less visible bleeding than non-smokers.
Why this happens: Smoking causes vasoconstriction (narrowing of blood vessels), which suppresses the normal bleeding response to inflammation. This masks the disease. Diagnosis often comes too late, after serious damage occurs.
Smoking also weakens immune response and interferes with normal gum tissue cell function.
Hormonal Changes
Hormonal fluctuations significantly increase gum sensitivity to plaque. Between 35% and 100% of pregnant women experience pregnancy gingivitis, depending on the study.
Elevated estrogen and progesterone levels increase blood vessel permeability and modify immune response. This makes gums more susceptible to inflammation and bleeding even with relatively low plaque levels.
Similar sensitivities occur during:
- Puberty
- Menstruation
- Menopause
Medications and Dry Mouth
Saliva plays a protective role by buffering acids and physically clearing bacteria from your mouth. Hundreds of medications reduce salivary flow, increasing gingivitis risk.
Common medications that cause dry mouth:
- Antihistamines
- Blood pressure medications
- Antidepressants
- Diuretics
- Muscle relaxants
- Opioids
These drugs interfere with the nerve signals responsible for saliva secretion. The result? Ideal conditions for bacterial overgrowth.
Chronic Health Conditions
Diabetes: The relationship between diabetes and gingivitis is bidirectional. Children with Type 1 diabetes show greater gum inflammation than non-diabetics with similar plaque levels. Hyperglycemia impairs immune response and healing, leading to heightened inflammation.
Immunocompromised states: Conditions like HIV/AIDS, leukemia, and cancer treatments lower immunity, increasing both the risk and severity of gingivitis.
Nutritional Deficiencies and Poor Diet
Vitamin C deficiency impairs collagen synthesis and compromises connective tissue integrity, leading to increased gingival bleeding and inflammation.
High-sugar diets fuel bacterial growth. A systematic review found that restricting free sugars significantly reduced gingival inflammation, with sugar feeding the acidogenic bacteria in plaque.
Early Warning Signs of Gingivitis
Recognizing symptoms early enables prompt treatment. Gingivitis is often painless, so visual and tactile signs become your primary indicators.
| Feature | Healthy Gums | Inflamed Gums (Gingivitis) |
|---|---|---|
| Color | Pink (or pigmented) | Red or reddish-purple |
| Texture | Firm, stippled (orange-peel texture) | Swollen, puffy, soft, shiny/smooth |
| Bleeding | No bleeding during care | Bleeds easily during brushing/flossing |
| Odor | Neutral | Persistent bad breath |
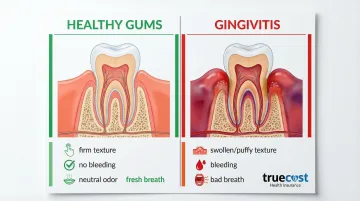
Red, Swollen, or Puffy Gums
Healthy gums are firm and pale pink (or naturally pigmented in darker skin tones). Inflamed gums appear red or purple and feel soft or swollen. Inflammation typically appears first between teeth and along the gumline, where plaque accumulates most easily.
Bleeding Gums During Brushing or Flossing
Bleeding gums signal active inflammation and should never be ignored. This is a primary clinical sign that requires attention.
Common scenarios include:
- Pink-tinged toothpaste when spitting
- Blood on dental floss
- Bleeding when eating certain foods
Many people mistakenly believe occasional bleeding is normal, but it isn't. Bleeding during routine oral care indicates inflammation requiring attention.
Persistent Bad Breath (Halitosis)
Bacterial buildup produces compounds that cause chronic bad breath. Unlike temporary food-related odor, this persistent smell returns quickly after mints or mouthwash because the underlying bacterial infection remains untreated.
Gum Tenderness or Sensitivity
You may experience:
- Discomfort when touching your gums
- Sensitivity to hot or cold foods
- Pain when chewing
Receding Gumline or Teeth Appearing Longer
While minor recession can occur with gingivitis, significant recession indicates progression toward periodontitis. If your teeth suddenly appear longer or you notice exposed tooth roots, seek immediate dental evaluation—this suggests the disease has advanced beyond the reversible stage.
How to Reverse Gingivitis
The good news: gingivitis is completely reversible with consistent action. Here's your step-by-step reversal plan.
Professional Dental Cleaning
Hardened tartar cannot be removed by brushing alone. A dentist or hygienist uses specialized instruments for:
- Scaling: Removing plaque and tartar from above and below the gumline
- Root planing: Smoothing root surfaces to prevent bacterial adhesion (if needed)
- Polishing: Removing surface stains and making teeth smoother
Scheduling guidelines:
- Book immediately upon diagnosis
- Standard maintenance: every 6 months
- High-risk patients (smokers, diabetics, history of gum disease): every 3-4 months
Proper Brushing Technique (Twice Daily)
Follow these specific instructions:
- Use a soft-bristled brush (hard bristles damage gum tissue)
- Position the brush at a 45-degree angle to your gumline
- Use gentle circular motions or short back-and-forth strokes
- Brush for 2 minutes (set a timer if needed)
- Cover all surfaces: outer, inner, and chewing surfaces
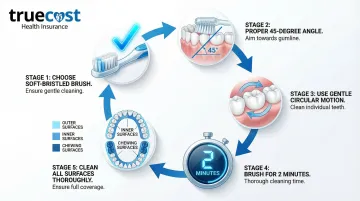
Proper technique removes plaque without damaging delicate gum tissue.
Daily Flossing
Flossing removes plaque and food particles from between teeth where toothbrush bristles cannot reach—where gingivitis often starts.
Technique:
- Use 18 inches of floss, winding most around your middle fingers
- Hold the floss taut between your thumbs and forefingers
- Curve the floss around each tooth in a C-shape
- Slide it gently beneath the gumline
- Use a clean section of floss for each tooth
Antiseptic Mouthwash
Beyond mechanical cleaning, antimicrobial mouthwashes reduce bacteria and reach areas brushing and flossing miss.
High-quality evidence shows chlorhexidine mouthrinse significantly reduces plaque and gingivitis over 4-6 weeks. However, long-term use (over 4 weeks) can cause tooth staining, so use it only as directed by your dentist.
Alternatively, mouthrinses containing eucalyptol, menthol, methyl salicylate, and thymol have demonstrated clinically significant benefits in long-term studies (6 months).
Look for ADA-accepted products for proven effectiveness.
Lifestyle Modifications
Quit smoking or tobacco use: Smoking is one of the most significant risk factors. Resources like state quitlines (1-800-QUIT-NOW) and smoking cessation programs can help.
Improve your diet:
- Reduce sugar and refined carbohydrates
- Increase vitamin C-rich foods (citrus fruits, berries, leafy greens)
- Stay hydrated to maintain saliva production
Manage chronic conditions: Work with your doctor to control diabetes and other conditions that increase gingivitis risk. Many ACA marketplace and Medicare Advantage plans include preventive dental benefits that cover professional cleanings—contact a licensed advisor to explore coverage options that support your oral health.
Reversal Timeline
With consistent care, healthy gum tissue can begin returning within days or weeks. Most people see:
- Initial improvement: Within 1-2 weeks of proper care
- Full reversal: Several weeks to months, depending on severity and adherence
Long-Term Prevention and Control Strategies
Prevention requires ongoing commitment to oral health habits:
Maintain your daily routine:
- Brush twice daily for 2 minutes
- Floss once daily
- Use antimicrobial mouthwash as recommended
Schedule regular dental visits: The CDC and ADA recommend checkups at least once a year, though most dentists suggest every 6 months.
If you have risk factors (diabetes, smoking history, previous gum disease), you may need more frequent visits—every 3-4 months.
Make preventive care accessible: Comprehensive health insurance plans now often include dental coverage that makes preventive care more affordable. Many **Medicare Advantage and ACA marketplace plans**—like those available through TrueCost Group—offer dental benefits covering routine cleanings and periodontal care.
This coverage removes financial barriers to the regular dental visits that prevent gingivitis progression.
Frequently Asked Questions
What is the main cause of gingivitis?
Plaque buildup from inadequate oral hygiene is the primary cause. When plaque isn't removed through daily brushing and flossing, bacteria accumulate and infect gum tissue, causing inflammation.
How do you get rid of gingivitis?
Gingivitis requires professional dental cleaning to remove hardened tartar, followed by improved at-home care—brushing twice daily, flossing once daily, and using antiseptic mouthwash as directed.
What does stage 1 gingivitis look like?
Early gingivitis presents with red, swollen gums that bleed easily during brushing or flossing. You may also notice mild tenderness and persistent bad breath that doesn't improve with mints.
Can gingivitis resolve itself?
No, gingivitis will not resolve without intervention. Improved oral hygiene is required to remove the bacterial plaque causing inflammation. However, the good news is that gingivitis is completely reversible with proper care—unlike advanced periodontal disease, which causes permanent damage.
How long does it take to reverse gingivitis?
With consistent proper care, gingivitis symptoms typically improve within 1-2 weeks. Full reversal—meaning complete restoration of gum health—often takes several weeks to months depending on severity and how consistently you follow your oral hygiene routine and professional care recommendations.
Is gingivitis contagious?
The bacteria that cause gingivitis can be transmitted through saliva, but gingivitis itself isn't contagious like a cold. Developing the condition requires plaque buildup and inadequate oral hygiene, not just bacterial exposure.
