Introduction
Picture this: it's 2 AM, and a throbbing toothache jolts you awake. The pain radiates from your jaw to your ear, and you're faced with a critical decision — can this wait until morning, or do you need to head to the ER right now?
A dental abscess is a bacterial infection that forms a pocket of pus near your tooth root or gums. What starts as a painful inconvenience can escalate into a life-threatening emergency within days.
Picture this: it's 2 AM, and a throbbing toothache jolts you awake. The pain radiates from your jaw to your ear, and you're faced with a critical decision — can this wait until morning, or do you need to head to the ER right now?
A dental abscess is a bacterial infection that forms a pocket of pus near your tooth root or gums. What starts as a painful inconvenience can escalate into a life-threatening emergency within days.
Many Americans delay dental care over cost concerns — but recognizing the difference between early symptoms and true emergency warning signs can save your tooth, and in serious cases, your life. This guide breaks down exactly what to watch for.
TLDR
- A dental abscess is a bacterial infection causing a pocket of pus that will never resolve without professional treatment
- Symptoms range from persistent toothache and gum swelling to facial swelling, fever above 100.4°F, and difficulty swallowing
- Go to the ER immediately if you experience breathing difficulty, neck swelling, or inability to swallow — these signal life-threatening spread
- Untreated infections can progress to Ludwig's angina, sepsis, or brain infections, all requiring hospitalization
- Many Americans qualify for ACA health plans that cover emergency room visits and dental benefits, often starting at $0/month
What Is a Dental Abscess and Why Does Timing Matter?
A dental abscess is a pocket of pus caused by bacterial infection that forms in or around your tooth. Two distinct types can develop, each affecting a different part of the mouth:
Periapical abscess occurs at the tip of the tooth root, typically resulting from untreated cavities or dental trauma. This type is more common in children but can affect anyone with tooth decay.
Periodontal abscess develops in the gum tissue alongside the tooth root, usually stemming from gum disease or poor oral hygiene. Adults experience this type more frequently.
Both types share one critical trait: neither will heal without treatment. Understanding which type you're dealing with helps explain why the infection can escalate so quickly.
Why Immediate Action Matters
A dental abscess will not resolve on its own — even when the pain suddenly stops. Many people assume pain relief means the infection cleared up. It doesn't. When the pain disappears, it typically means the tooth nerve has died, while bacteria continue spreading silently into surrounding bone and soft tissue.
The infection follows a predictable path: tooth → jaw → neck → bloodstream. Each stage left untreated carries more serious consequences than the last.
Common Causes
Understanding what causes dental abscesses helps you assess your risk:
- Untreated cavities — decay erodes tooth enamel, creating a pathway for bacteria to reach the pulp
- Cracked or chipped teeth — trauma provides direct bacterial access to the tooth interior
- Failed dental procedures — previous root canals or fillings can sometimes allow reinfection
- Poor dental hygiene — plaque and tartar buildup contribute to both tooth decay and gum infections
Dental Abscess Symptoms: Recognizing the Stages
Symptoms typically follow a progression from mild to severe. Identifying which stage you're experiencing determines how urgently you need professional care.
Early-Stage Symptoms
The initial warning signs indicate a dental infection is forming:
- Persistent throbbing or sharp toothache that doesn't go away
- Sensitivity to hot or cold foods and beverages
- Pain when biting down or chewing
- The affected tooth feels slightly raised or loose in its socket
These symptoms warrant scheduling a dentist appointment within 1-2 days. Don't ignore these signs or manage them indefinitely with painkillers. The infection will progress without professional drainage and treatment.
Moderate Symptoms Requiring Prompt Dental Care
As the infection advances, symptoms become more visible and uncomfortable:
- Swelling in the gum or cheek near the affected tooth
- Redness and tenderness around the tooth
- Visible gum boil (parulis) — a soft, pimple-like bump on the gum that may drain pus
- Bad taste in the mouth from draining infection
- Swollen lymph nodes in your neck or under your jaw
Critical thresholds: According to ADA clinical guidelines, an abscess larger than 1 cm in diameter or a fever above 100.4°F (38°C) means you need to be seen by a dentist the same day or within 24 hours — not next week.
Severe Symptoms That Signal a Spreading Infection
These symptoms indicate the infection has begun spreading beyond the tooth into deep tissue:
- High fever with chills — body temperature above 100.4°F with systemic illness
- Facial swelling extending to your eye, jaw, or cheek
- Trismus (lockjaw): inability to open your mouth more than two fingers wide
- Difficulty swallowing as the infection reaches throat structures
- Visible swelling under your chin or along your neck

At this stage, the infection may be entering the deep tissue spaces of your head and neck. This is a medical emergency requiring immediate hospital care.
When to Seek Immediate Emergency Treatment
Some dental abscess symptoms require a hospital ER — not a dentist's office. ER doctors can stabilize the infection with IV antibiotics and manage your airway immediately if the situation becomes dangerous.
Go to the ER Immediately If You Experience
The following are non-negotiable red flags, per clinical guidance from the Mayo Clinic:
- Difficulty breathing or shortness of breath
- Difficulty swallowing or inability to drink liquids
- Severe swelling of the neck, floor of the mouth, or around the eyes
- Inability to open your mouth more than two fingers wide
- Severe pain unresponsive to maximum doses of over-the-counter painkillers
Each of these symptoms can signal a life-threatening complication:
| Condition | What It Is | Why It's Dangerous |
|---|---|---|
| Ludwig's angina | Rapidly spreading infection of the floor of the mouth | Can obstruct your airway; mortality historically exceeded 50%, now ~8% with modern treatment |
| Cavernous sinus thrombosis | Infection spreading to blood vessels at the base of the skull | Dental infections cause ~7% of cases; can lead to stroke or death |
| Sepsis | Infection entering the bloodstream | Triggers a systemic inflammatory response that can cause organ failure |
Important: ER doctors cannot perform dental procedures like root canals or extractions, but they will administer IV antibiotics, manage your airway, and provide pain control until you can see a dentist. This stabilization is still critical and potentially life-saving care.
Call a Dentist the Same Day If You Experience
These symptoms don't require the ER but cannot wait for a regular appointment:
- Abscess larger than 1 cm (about half an inch)
- Fever above 38°C (100.4°F)
- Visible hard lump or severe swelling on your face or jaw
- Tender or swollen lymph nodes in your neck
If you cannot reach your regular dentist, call an urgent care clinic or dental emergency line. Most areas have after-hours dental emergency services available — search for "emergency dentist" plus your city name.
What Happens When You Delay Treatment
Between 2020 and 2022, tooth disorders accounted for an annual average of 1.94 million emergency department visits in the U.S., with approximately 80% of these visits for preventable conditions like abscesses. Many of these ER visits could have been managed earlier with routine dental care, at a fraction of the cost.
The Dangerous Illusion of Pain Relief
Many people delay care because the pain temporarily stops. This is one of the most dangerous misconceptions about dental abscesses. When the tooth nerve dies, pain disappears, but the bacterial infection continues to progress and spread into surrounding bone and soft tissue. You feel better, but the infection is actually worsening.
The Progression of Untreated Infection
Without treatment, dental infections follow a predictable and increasingly serious path:
- Localized abscess — infection contained within or immediately around the tooth
- Cellulitis — infection spreads to skin and soft tissue, causing visible facial swelling
- Osteomyelitis — infection reaches the jawbone, causing bone deterioration
- Ludwig's angina or parapharyngeal abscess — infection spreads to deep neck spaces, threatening the airway
- Sepsis or cavernous sinus thrombosis — infection enters the bloodstream or reaches the brain
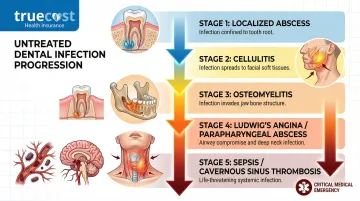
Treatment at stage one typically means a drainage procedure and antibiotics. By stage four or five, it means hospitalization, ICU care, and surgeries that can cost tens of thousands of dollars.
Oral Health Consequences
The systemic risks get the most attention, but the damage to your mouth is just as lasting:
- The affected tooth may become impossible to save, leading to extraction
- Bone loss in the jaw can complicate or disqualify you from implants and other restorative work
- Neighboring healthy teeth can sustain root damage from spreading infection
Caught early, most abscesses are treatable with a root canal or simple drainage — procedures that preserve the tooth and prevent months of costly follow-up care.
What to Do While Waiting for Care — and How to Afford It
If you're waiting for a dental appointment (not experiencing emergency symptoms), these safe temporary measures can help manage pain:
Safe pain management:
- Warm saltwater rinses (½ teaspoon salt in 8 oz warm water, swish gently)
- Over-the-counter pain relievers: ibuprofen (Advil) or acetaminophen (Tylenol) per labeled dosing
- Avoid very hot or cold foods that trigger sensitivity
- Sleep with your head elevated to reduce pressure and throbbing
These are NOT substitutes for treatment — they only provide temporary relief while you arrange professional care.
What to Avoid
Never attempt these dangerous "home remedies":
- Do not try to drain the abscess yourself — this can introduce new bacteria and cause serious complications
- Do not rely on numbing gels long-term — they mask symptoms without addressing the infection
- Do not assume the problem is resolved if pain subsides — remember, pain relief often means nerve death, not infection resolution
Addressing the Cost Barrier
Cost is often why people attempt dangerous home remedies instead of seeking care. But delaying treatment can turn a $200 dentist visit into a $749 ER visit — or a hospitalization costing far more.
ACA marketplace plans and Medicare Advantage plans — including options through TrueCost Group — offer real coverage for these situations. According to TrueCost Group, 80% of their clients qualify for full coverage plans starting at $0/month, with most paying between $0–$50 monthly.
These plans typically cover:
- Emergency room and urgent care visits
- Primary doctor and specialist visits
- Prescription medications and pre-existing conditions
- Supplemental dental, vision, and hearing (on select plans)

Don't avoid care because of cost. Explore your coverage options before a manageable dental problem becomes a life-threatening emergency. TrueCost Group's licensed advisors can help you find a plan that fits your situation — reach them at 1-888-788-8285 or info@truecostgroup.com.
Frequently Asked Questions
Can a dental abscess go away on its own?
No. A dental abscess will never resolve without professional treatment. Even if pain stops due to nerve death, the bacterial infection continues spreading and can become life-threatening without drainage and antibiotics.
What happens if a tooth abscess is left untreated?
Untreated abscesses can spread to your jaw, neck, and bloodstream, causing dangerous conditions like Ludwig's angina, osteomyelitis, or sepsis — each requiring hospitalization and significantly harder to treat than the original abscess. Tooth loss and jawbone deterioration are also likely outcomes.
How do I know if my tooth abscess is spreading?
Watch for these warning signs — all require emergency care:
- Swelling spreading to your face, neck, or under your chin
- Fever
- Difficulty swallowing or opening your mouth
- Feeling severely unwell overall
Can I go to the ER for a tooth abscess?
Yes, the ER is appropriate when severe symptoms are present: breathing difficulty, inability to swallow, neck swelling, or uncontrollable pain. ER doctors will administer IV antibiotics and pain management but cannot perform dental procedures, so follow-up with a dentist is still required.
How long does it take for a dental abscess to become dangerous?
There is no predictable timeline. A dental infection can spread over days, weeks, or even months, depending on your immune system and the bacteria involved. This is why prompt evaluation is always recommended rather than waiting for symptoms to worsen.
What is the difference between a tooth infection and a tooth abscess?
All tooth abscesses are infections, but not all tooth infections form an abscess. An abscess specifically refers to a localized pocket of pus, representing a more advanced stage of infection that always requires professional drainage.