Introduction
You're lying awake at 2 AM with throbbing tooth pain that won't quit. By morning, your dentist delivers the news: you need a root canal. For many people, those three words trigger instant anxiety.
Here's the truth: modern root canals are far from the nightmare you've heard about. Thanks to advanced anesthesia and refined techniques, most patients report that the experience feels no worse than getting a routine filling. The real pain comes from the infection itself—not the treatment that fixes it.
This guide covers everything you need to know: how the procedure works, what pain levels to expect, cost breakdowns with insurance, signs you need treatment, and what recovery looks like.
By the end, you'll understand why saving your natural tooth is worth it.
TL;DR
- Root canal removes infected pulp, cleans canals, and seals the tooth to prevent reinfection
- Modern techniques make it as comfortable as a filling—90% of patients pain-free within a week
- Costs range from $700-$1,500 depending on tooth type, with insurance typically covering 50-80%
- Watch for severe tooth pain, prolonged hot/cold sensitivity, swollen gums, or visible abscesses
- With proper restoration and care, treated teeth can last a lifetime
What Is a Root Canal?
A root canal is a dental procedure that removes infected or inflamed tissue from inside your tooth. Despite its intimidating reputation, it's a routine treatment designed to save your natural tooth rather than extract it.
Understanding Tooth Anatomy
Your tooth has three main layers:
- Enamel: The hard outer shell that protects the tooth
- Dentin: The middle layer beneath the enamel
- Pulp: The soft inner tissue containing nerves, blood vessels, and connective tissue
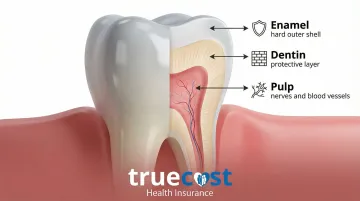
When bacteria penetrate through decay or cracks, they reach the pulp chamber and trigger infection. This causes inflammation, severe pain, and potential abscess formation.
The Goal of Treatment
Root canal therapy eliminates the infection and seals the tooth to prevent bacteria from re-entering. Here's what makes it possible: once your tooth is fully developed, it can survive without the pulp because surrounding tissues continue to nourish it.
Preserving your natural tooth structure offers significant advantages over extraction:
- Maintains normal bite force and chewing function
- Prevents adjacent teeth from shifting out of position
- Eliminates the need for costly replacements like implants or bridges
How it differs from alternatives:
- Extraction: Removes the entire tooth, causing bone loss and requiring replacement
- Implants: Cost 2-3 times more than root canals while replacing (not saving) your natural tooth
- Root canal: Preserves your natural tooth with a 97% survival rate after 10 years
Signs You Need a Root Canal
Recognizing the warning signs early can prevent complications and potentially save your tooth. The American Association of Endodontists identifies these key symptoms:
Primary warning signs:
- Severe, persistent pain when chewing or applying pressure to the tooth
- Prolonged sensitivity to hot or cold that lingers after the stimulus is removed
- Darkened or discolored tooth indicating internal damage or dying pulp
- Swollen or tender gums near the affected tooth
- Pimple-like bump on gums (called a fistula or abscess) that may ooze pus
With more than 15 million root canal procedures performed annually in the United States, this treatment has become a cornerstone of modern dental care. That's over 41,000 procedures every day—yet many of these could have been simpler interventions if caught earlier.
The Silent Infection Problem
Sometimes infection develops without obvious symptoms—no pain, no swelling, no visible signs, yet the damage continues beneath the surface. This is why regular dental checkups matter, as your dentist can detect problems through X-rays before you ever feel discomfort.
Early detection benefits:
- Simpler treatment procedures
- Better long-term outcomes
- Lower overall costs
Why Root Canals Are Necessary
Ignoring an infected tooth isn't an option. Without treatment, the consequences escalate quickly and can affect your overall health.
Common Causes of Pulp Damage
Three primary factors lead to root canal needs:
- Deep decay that penetrates through enamel and dentin to reach the pulp
- Cracks or chips that expose the pulp chamber to bacteria
- Trauma or injury that damages the tooth's internal structure
Once bacteria invade the pulp, infection spreads through the root canal system. The pulp tissue dies (necrosis), and an abscess forms at the root tip.
The infection destroys surrounding bone and can spread to adjacent teeth or even into your bloodstream.
Success Rates: Root Canal vs. Extraction
The clinical data strongly favors saving your natural tooth. Long-term studies show impressive survival rates for root canal-treated teeth:
| Time Period | Survival Rate |
|---|---|
| 5 years | 93% |
| 10 years | 97% |
| 20 years | 81% |
When comparing root canal treatment to extraction followed by an implant, both options show high survival rates. However, root canals require fewer follow-up interventions—implants have a 12.4% re-intervention rate compared to just 1.3% for root canal treatments.
Why Saving Your Natural Tooth Matters
Preserving your natural tooth provides distinct advantages:
- Maintains your natural bite force and chewing efficiency
- Prevents adjacent teeth from shifting out of position
- Preserves jawbone density (extraction leads to bone resorption)
- Costs significantly less than extraction plus replacement
- Retains the natural periodontal ligament that helps you sense pressure
Placing a crown after root canal treatment significantly improves longevity—extending median survival time by 5.3 years compared to teeth without crowns.
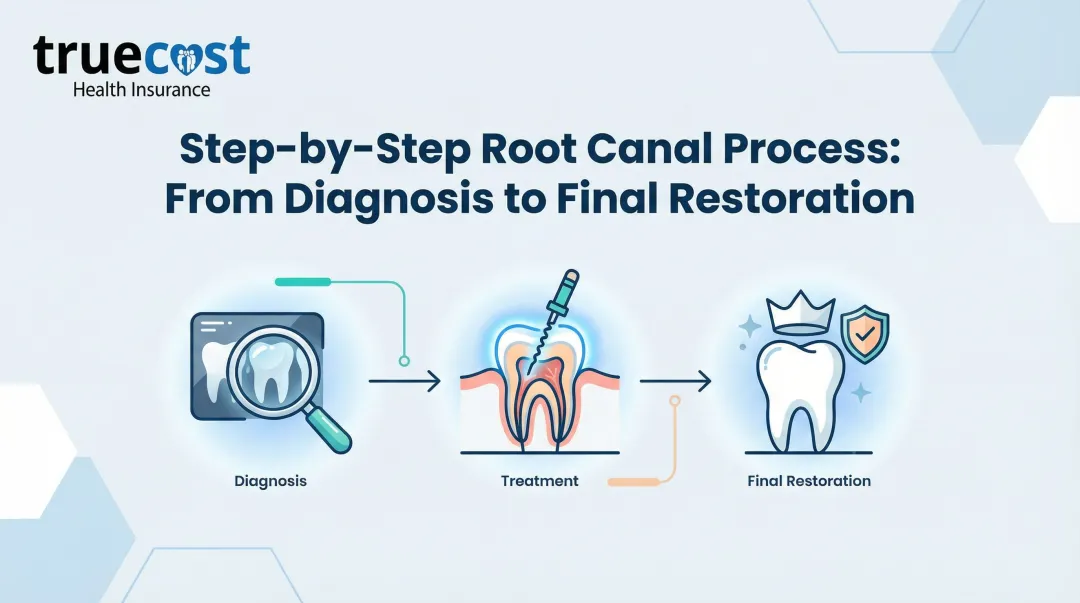
How the Root Canal Procedure Works (Step-by-Step)
Most root canal treatments are completed in one or two appointments, with each visit lasting approximately 90 minutes. Research confirms that single-visit treatments are as effective as multi-visit approaches for most cases.
Step 1: Examination and X-Rays
Your dentist or endodontist takes detailed X-rays to evaluate the extent of infection and plan the treatment approach.
These images show the shape of your root canals and whether infection has spread to surrounding bone.
Step 2: Anesthesia and Isolation
The procedure begins with:
- Local anesthesia that numbs the tooth and surrounding area completely
- Pressure sensations during treatment, but no sharp pain
- A rubber dam (protective sheet) placed around the tooth to keep it dry and isolated from saliva
Step 3: Accessing the Pulp Chamber
The dentist creates a small opening in the crown of your tooth to access the infected pulp chamber. For front teeth, the opening is made on the back surface. For molars, it's made on the chewing surface.
Step 4: Cleaning and Shaping
This is the core of the procedure. Using specialized instruments, the dentist:
- Removes all infected and inflamed pulp tissue
- Cleans the interior canal walls thoroughly
- Disinfects the canals with antimicrobial solutions
- Shapes the canals to prepare them for filling
Step 5: Filling and Sealing
The cleaned canals are filled with a biocompatible rubber-like material called gutta-percha. This material is sealed with adhesive cement to prevent bacteria from re-entering. A temporary filling closes the access opening.
Step 6: Final Restoration
Because the temporary filling provides only short-term protection, you'll return to your general dentist for a permanent crown or filling. This restoration protects the tooth from fracture and restores full function. The permanent restoration is essential—without it, the treated tooth remains vulnerable to damage.
Pain Level: What to Expect During and After
The biggest myth about root canals? That they're incredibly painful. Modern root canal treatment is far more comfortable than most people expect.
During the Procedure
Thanks to local anesthesia, you should feel little to no pain during treatment. The experience is comparable to getting a routine filling—you may feel pressure or vibration from the instruments, but not sharp pain.
If you do experience discomfort, tell your dentist immediately. They can administer additional anesthesia to ensure you remain comfortable throughout the procedure.
Most patients worry more about the procedure itself than recovery, but understanding what comes next helps you prepare.
After the Procedure
Clinical studies show that post-treatment pain is typically mild and short-lived:
- Pain levels decrease significantly within 24 hours
- Nearly 90% of patients report being pain-free within one week
- Most people manage discomfort with over-the-counter pain relievers like ibuprofen
Normal post-treatment sensations:
- Mild soreness or tenderness for 2-4 days
- Slight sensitivity when biting down
- Dull ache as inflammation subsides
The key takeaway? The infection causes the severe pain—not the treatment that eliminates it.

Debunking the Pain Myth
Root canal therapy actually relieves the pain you've been experiencing. Modern techniques, refined instruments, and effective anesthesia have transformed this procedure into a routine, relatively comfortable experience.
If cost concerns are preventing you from getting needed dental work, many health insurance plans include dental coverage or supplemental dental benefits. TrueCost Group can help you explore options that make preventive and restorative dental care more accessible.
Root Canal Cost and Insurance Coverage
Cost Ranges by Tooth Type
Root canal costs vary based on tooth complexity and location. National averages break down by tooth type:
| Tooth Type | Cost Range | Why It Varies |
|---|---|---|
| Front tooth (incisor) | $700-$1,000 | Single canal, easier access |
| Premolar | $800-$1,200 | One or two canals |
| Molar | $1,200-$1,500+ | Multiple canals, more complex |
The overall average cost is approximately $1,165, with a typical range of $500-$1,800 before insurance.
Factors That Affect Price
Several variables influence your final bill:
- Tooth location: Molars cost more due to multiple canals and difficult access
- Infection severity: Extensive infections may require additional appointments
- Provider type: Endodontists (specialists) may charge 50% more than general dentists
- Geographic location: Urban areas typically have higher costs than rural regions
Insurance Coverage
Most dental insurance plans classify root canals as either "Basic" or "Major" services. Coverage typically ranges from 50-80% after your deductible is met.
Here's what major carriers typically cover:
- Delta Dental PPO: 50-80% depending on plan tier
- Aetna DMO: 80% for front teeth, 50% for molars
- Cigna DPPO: 50-80% as basic restorative service
- UnitedHealthcare PPO: 80% as basic dental service
Keep in mind: most plans have annual maximum benefits of $1,000-$2,000. A root canal plus crown can quickly exhaust this limit.
For Those Without Dental Coverage
Without dental insurance, ACA marketplace health plans may include dental benefits as part of your coverage.
TrueCost Group specializes in connecting individuals with ACA marketplace plans that include dental coverage. 80% of clients qualify for plans starting at $0/month, with most people paying between $0-$50/month for comprehensive coverage. Call 1-888-788-8285 to check your eligibility.
Cost Comparison: Root Canal vs. Alternatives
Saving your tooth is almost always more cost-effective than extraction plus replacement:
| Treatment Option | Total Cost | Long-Term Considerations |
|---|---|---|
| Root canal + crown | $1,500-$3,000 | Preserves natural tooth; high success rate |
| Extraction only | $100-$500 | Leads to bone loss and tooth shifting |
| Extraction + implant | $3,100-$5,500+ | 2-3x more expensive; longer treatment time |
| Extraction + bridge | $1,600-$3,000+ | Requires altering adjacent healthy teeth |

Recovery and Aftercare
Most patients return to normal activities the same day or the next day after treatment, with full healing typically taking 1-2 weeks.
Immediate Aftercare (First 24-48 Hours)
- Don't chew on the treated tooth until you receive your permanent crown or filling
- Eat soft foods for the first few days to avoid putting pressure on the tooth
- Avoid extremely hot or cold foods temporarily to minimize sensitivity
- Don't smoke or drink hot liquids for at least the first hour after treatment
Daily Care During Healing
- Brush and floss normally, but be gentle around the treated area
- Take prescribed antibiotics exactly as directed (if given)
- Use over-the-counter pain relievers as needed for mild discomfort
- Rinse with warm salt water to soothe gums
When to Call Your Dentist
While mild discomfort is normal during healing, contact your dental office immediately if you experience:
- Severe pain lasting more than a few days
- Visible swelling inside or outside your mouth
- Allergic reaction to medication (rash, itching, difficulty breathing)
- Uneven bite or feeling that your temporary filling is too high
- Loss of the temporary filling or crown
Long-Term Success
With proper restoration and oral hygiene, root canal-treated teeth often last a lifetime. Clinical data shows:
- 97% of treated teeth remain functional after 10 years
- 81% survive for 20 years or longer
Keys to long-term success:
- Complete the final restoration promptly (don't delay getting your crown)
- Maintain excellent oral hygiene with regular brushing and flossing
- Attend routine dental checkups every six months
- Address any new decay or damage immediately
Alternatives to Root Canals
While root canal treatment is often the best option, extraction is sometimes necessary.
When Extraction Might Be Recommended
Dentists typically recommend extraction when:
- The tooth is severely fractured beyond repair
- There's insufficient bone support due to advanced gum disease
- The root structure is too damaged or complex to treat effectively
- Cost constraints make restoration financially impossible
The Biological Cost of Extraction
Before choosing extraction, understand the long-term impact on your jaw. Research shows that within the first three months after extraction, the jawbone loses up to 40% in height and 60% in width if the site isn't preserved.
Additional consequences include:
- Adjacent teeth shift into the empty space, altering your bite
- Opposing teeth can over-erupt, creating alignment problems
- Bone loss continues progressively over time
- Facial structure may change with extensive bone loss
Replacement Options After Extraction
If you choose extraction, you'll need to replace the tooth to maintain function. Replacement costs vary significantly, and some health insurance plans may cover portions of these procedures:
Dental implant ($3,000-$5,000): A titanium post surgically placed in the jawbone and topped with a crown. This option prevents bone loss and functions like a natural tooth, though it costs significantly more than root canal treatment.
Fixed bridge ($1,500-$2,500): A prosthetic tooth anchored to adjacent teeth. This requires grinding down healthy neighboring teeth, which weakens them permanently.
Partial denture ($300-$5,000): A removable appliance that fills the gap. This is the least expensive option but also the least stable, requiring regular adjustments.
Many health insurance plans include dental benefits that can help offset these costs. If you're uninsured or underinsured, checking your eligibility for comprehensive coverage can make these treatments more affordable.
Frequently Asked Questions
What is a root canal and what happens during the procedure?
A root canal removes infected pulp tissue from inside your tooth, cleans the interior canals, and seals them with a rubber-like material. The tooth is then restored with a crown or filling to protect it and restore function.
How long do root canals last?
With proper care and restoration, most root canal-treated teeth last a lifetime. Clinical studies show 97% survival rates at 10 years and 81% at 20 years. Success depends on getting a permanent crown promptly and maintaining excellent oral hygiene.
What are the signs that I need a root canal?
Key symptoms include severe tooth pain when chewing, prolonged sensitivity to hot or cold, swollen gums, darkened tooth color, or a pimple-like bump (abscess) on your gums. Sometimes there are no symptoms, which is why regular dental checkups are essential.
Do you need a crown after a root canal?
Crowns are typically recommended for molars and premolars because these teeth endure significant chewing forces and the root canal procedure removes substantial tooth structure. Front teeth (incisors) may only require a filling if enough natural tooth structure remains intact.
How much does a root canal cost?
Costs typically range from $700-$1,000 for front teeth, $800-$1,200 for premolars, and $1,200-$1,500+ for molars. Most dental insurance plans cover 50-80% of the procedure after your deductible, significantly reducing out-of-pocket expenses.
Is a root canal painful?
Modern anesthesia makes root canal treatment no more painful than getting a routine filling. You may feel pressure but shouldn't experience sharp pain. Mild soreness for 2-4 days is normal, and nearly 90% of patients are pain-free within one week.