A dental plan waiting period is simply the time between enrollment and when certain services become eligible for coverage. Most preventive care is covered right away, while basic and major procedures may require a few months.
Most plans require you to wait anywhere from 6 to 12 months before major services like crowns and root canals are covered. Basic cleanings usually start immediately, but the bigger treatments require patience.
The rules vary widely between carriers and plan types. The timing can feel frustrating when your tooth starts aching the week after you sign up. We'll break down the timeline for each category, show you what to expect, and help you avoid surprise bills.
Key Takeaways
Preventive care, like cleanings and exams, typically starts immediately with zero waiting time.
Major procedures, including crowns and root canals, usually require six to twelve months.
Most plans cap annual coverage at between $1,000 and $2,000 per year maximum.
HealthSpring PPO plans through TrueCost Group eliminate all waiting periods from day one.
You can visit dentists during waiting periods, but you may need to pay out of pocket for restricted services.
What Does a Waiting Period Mean on Dental Insurance?
A waiting period is the mandatory gap between when coverage begins and when specific benefits activate. Carriers use these windows to maintain plan stability and prevent people from enrolling only for immediate, expensive procedures. The length depends entirely on the type of dental work needed.
Different Types of Dental Insurance Waiting Periods
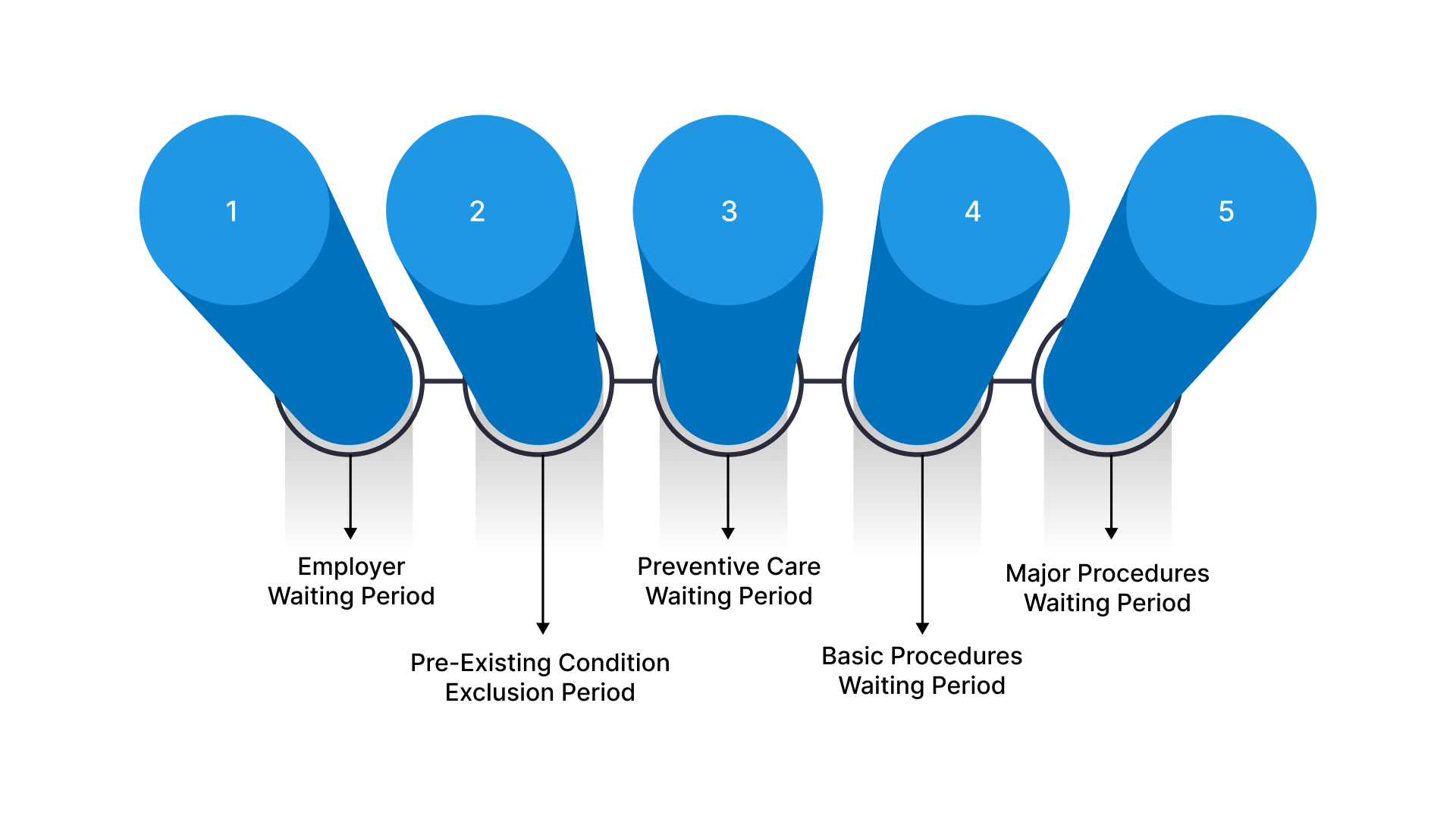
Plans structure waiting periods differently based on procedure complexity and enrollment circumstances. Here are the main categories:
Employer Waiting Period: Companies offering dental benefits often impose a waiting period from a few days to twelve months after hire. Check your specific coverage documents for exact timelines.
Pre-Existing Condition Exclusion Period: Insurance won't pay for treatment related to conditions diagnosed before enrollment during this window. This prevents people from buying coverage solely for known upcoming procedures. Simple issues like cavities typically get covered immediately, while complex treatments face longer waits.
Preventive Care Waiting Period: Routine exams, cleanings, and X-rays usually have zero waiting time. Coverage for these services activates on your enrollment date or shortly after.
Basic Procedures Waiting Period: Fillings, simple extractions, and similar treatments often require three to six months of active coverage. Some carriers reduce this window to 30 days.
Major Procedures Waiting Period: Crowns, bridges, dentures, root canals, and oral surgery typically require six to twelve months of enrollment. This represents the longest wait across all dental service categories.
Waiting six months for a crown when your tooth hurts today feels impossible. TrueCost Group can connect you with HealthSpring PPO plans that eliminate waiting periods entirely, so major procedures like root canals and bridges are covered from day one.
Get up to $5,000 in annual coverage, access to 85,000+ dentists nationwide, plus $200 vision and $500 hearing benefits included. No contracts, no confusing paperwork, no watching the calendar while dental problems get worse.
Contact TrueCost Group and start treatment this week, not next year.
Can I Visit a Dentist During the Waiting Period?
Yes, you can absolutely visit a dentist during the waiting period. Your coverage is active from day one for preventive services like cleanings, exams, and X-rays. These appointments cost nothing out of pocket on most plans, or you'll pay a small copay depending on your specific policy. The waiting period only restricts coverage for certain procedures, not your ability to seek care.
Visiting during this window helps in several ways:
Your dentist can identify issues early before they become emergencies.
You'll establish a relationship with a provider who knows your dental history.
Regular checkups prevent minor problems from escalating into major procedures that cost significantly more.
Even if a filling or crown gets recommended, having the diagnosis documented creates a clear timeline for when treatment becomes covered.
You'll simply pay out of pocket for any services still within their waiting period. Many dentists offer payment plans or discounted rates for uninsured procedures. Some patients may choose to delay non-urgent treatments until coverage kicks in.
Others proceed with necessary work immediately and absorb the cost. The choice depends on the severity of the issue and your financial situation.
Benefit Limitations in Dental Insurance Plans
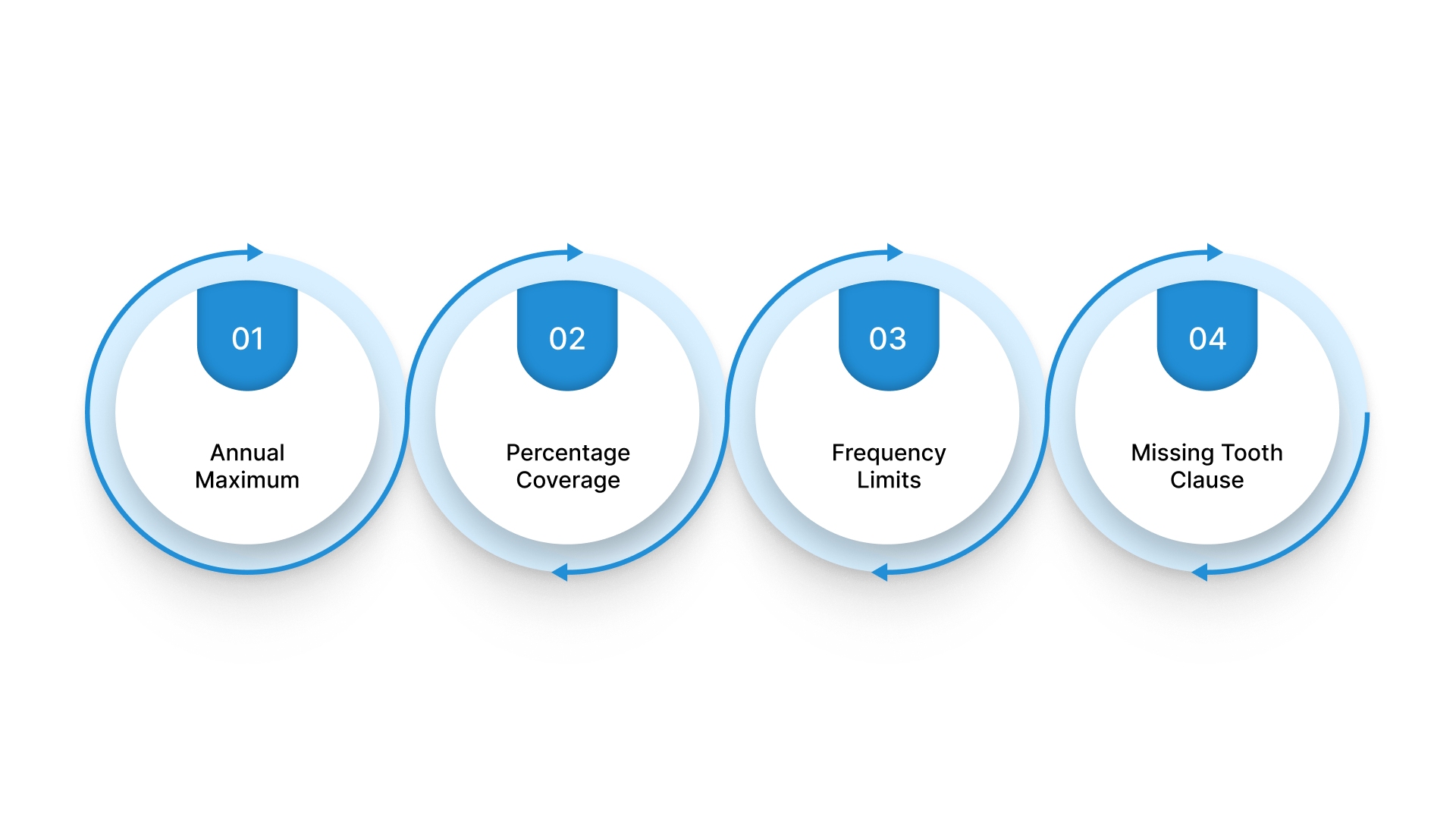
Even after waiting periods end, dental insurance often comes with caps on what it will pay. Understanding these limits helps you budget for treatments and avoid surprise bills when major work gets recommended.
Annual Maximum: Most plans cap total coverage between $1,000 and $2,000 per year, though some reach $5,000. Once you hit that limit, you pay 100% out of pocket for additional procedures until the next calendar year.
Percentage Coverage: Plans typically cover preventive care at 100%, basic procedures at 80%, and major work at 50%. This is known as the 100-80-50 coverage model. You're responsible for the remaining percentage even after meeting your deductible.
Frequency Limits: Cleanings usually get covered twice per year, X-rays once annually, and major procedures like crowns once every five years. Requesting treatment outside these windows means paying full price.
Missing Tooth Clause: Some policies won't cover replacement for teeth lost before enrollment. This exclusion can last indefinitely or for a specific period, depending on the carrier.
When Can You Waive the Dental Insurance Waiting Period?
Certain circumstances allow you to bypass the standard waiting periods and access full benefits immediately. These exceptions vary by carrier but follow common patterns across the industry.
Employer Group Plans: Switching from one employer dental plan to another often lets you carry over your creditable coverage. Provide proof of continuous enrollment to eliminate waiting periods for services already satisfied under your previous plan.
No-Waiting-Period Plans: Specialty carriers like HealthSpring offer plans designed without mandatory waiting periods. You'll pay slightly higher premiums in exchange for immediate access to major procedure coverage from enrollment day.
Special Enrollment Periods: Life events like marriage, birth, or loss of other coverage may trigger a special enrollment that waives certain restrictions. Check with your carrier within 30 days of the qualifying event.
TrueCost Group Eliminates the Wait with HealthSpring PPO
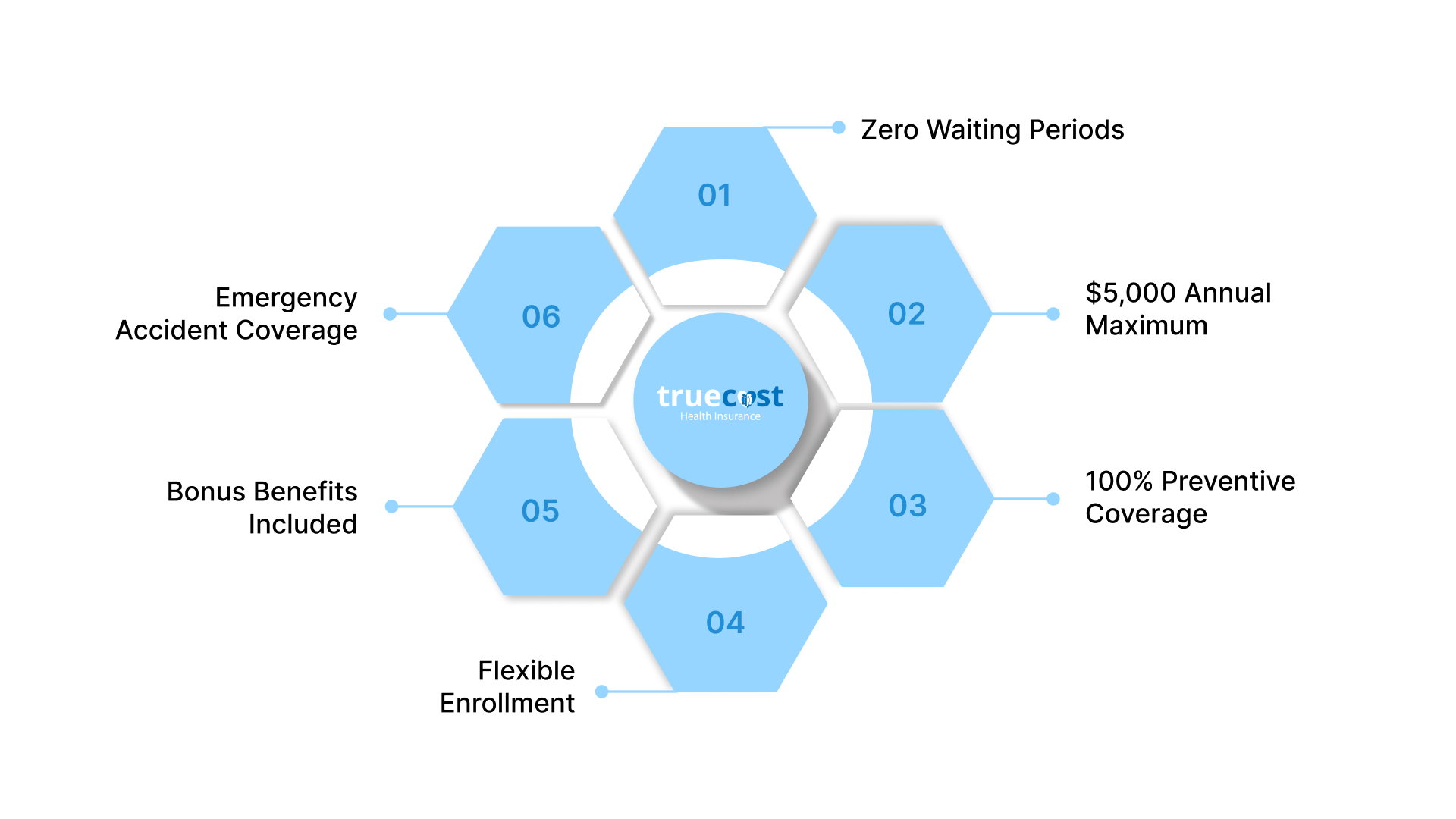
TrueCost Group partners exclusively with HealthSpring to deliver PPO dental coverage that works the moment you enroll. A PPO plan means you can choose any licensed dentist nationwide while enjoying negotiated discounts at over 85,000 in-network providers. Here's what sets HealthSpring apart:
Zero Waiting Periods: Major procedures like crowns, root canals, and bridges are covered immediately. No six-month countdown, no delayed treatment, no worsening dental problems while you wait.
$5,000 Annual Maximum: Access significantly higher coverage limits than standard plans that cap at $1,000 to $2,000 per year.
100% Preventive Coverage: Cleanings, exams, and X-rays cost nothing out of pocket from day one.
Flexible Enrollment: Sign up through WhatsApp or Facebook Messenger in minutes. Month-to-month terms mean no long-term commitment.
Bonus Benefits Included: Every plan comes with $200 vision and $500 hearing coverage at no extra cost.
Emergency Accident Coverage: An optional add-on protects you from unexpected dental injuries requiring immediate care.
Stop postponing the dental work you need. Connect with TrueCost Group and book your treatment this week with full coverage active.
Conclusion
Dental insurance waiting periods protect carriers while keeping premiums affordable for everyone enrolled. Most plans cover preventive care immediately and require three to twelve months for major procedures.
Knowing these timelines before you enroll prevents billing surprises and helps you plan treatments strategically. The right coverage gives you access to care when you need it, not months down the road.
Watching the calendar while a toothache gets worse shouldn't be part of getting insured. TrueCost Group can connect you directly with HealthSpring PPO plans that cover major dental work from day one, with no waiting periods required.
Talk to us today and schedule the treatment your teeth need this week, not six months from now.
Frequently Asked Questions
1. What is a dental plan waiting period?
A waiting period is the time between enrollment and when specific dental services become covered. Preventive care starts immediately, while major procedures typically require six to twelve months.
2. How long are dental insurance waiting periods?
Preventive services have zero wait time. Basic procedures like fillings need three to six months. Major work, including crowns and root canals, requires six to twelve months of enrollment.
3. Can I get dental work done during a waiting period?
Yes, you can visit dentists and receive any treatment needed. You'll simply pay out of pocket for services still within their waiting period until coverage activates.
4. Do all dental plans have waiting periods?
No. Most traditional plans impose waiting periods, but specialty carriers like HealthSpring offer zero-wait plans. These typically charge slightly higher premiums for immediate major procedure coverage.
5. How do I avoid dental insurance waiting periods?
Enroll in no-waiting-period plans through providers like HealthSpring. Alternatively, provide proof of prior creditable coverage when switching employer plans to waive certain waiting requirements.


