
Major dental care is one of those phrases that sounds clear until you try to use it. One plan calls crowns “major.” Another files the same crown under a different category. A dentist’s office might say your plan “takes it,” but your bill still changes if the dentist is out of network or the plan applies different rules for major services.
This guide keeps it simple and practical. You’ll learn what “major dental care” usually refers to, how it differs from basic and preventive categories, and why major work is where costs jump.
You’ll also get a short checklist to verify coverage before you schedule, so you don’t end up paying cash by accident when a plan option could have reduced your out-of-pocket.
Key Takeaways
Major dental care usually means larger restorations or tooth replacement, but the exact list is plan-defined.
The fastest way to avoid surprises is to confirm 3 things: whether the service is classified as major, whether your dentist is in-network, and whether a pre-treatment estimate is worth requesting.
“Major” is where out-of-pocket often spikes because of annual maximums, waiting periods, and plan limits or frequency rules.
A quick table can help you map common procedures to typical categories, then verify the label in your plan documents.
If you’re on a tight budget, the goal is simple: avoid paying cash by accident when a plan option could reduce out-of-pocket.
What Is Major Dental Care?
Major dental care usually means higher-complexity work that restores a tooth’s structure or replaces missing function, not routine maintenance.
The key point is category logic: insurance uses “major” as a billing bucket for services that often involve more chair time, more technique sensitivity, and sometimes lab fabrication or multiple visits. That’s why major services tend to sit under different plan rules than preventive or basic care.
Also, major ≠ urgent and major ≠ cosmetic. A procedure can be major because it’s complex or restorative, even if it’s planned. And something cosmetic may not be covered at all, even if it’s expensive.
If you want the simplest way to use the term correctly, major dental care is whatever your plan lists under “Major Services,” “Major Restorative,” or similar language in the benefits summary, because that label is what drives how the claim is processed.
What Dental Services Are Usually Considered Major?
Most plans use “major” for bigger restorative and replacement work. The exact grouping can still vary, but these are the procedures that most often show up in the major bucket:
Crowns (including many full-coverage restorations)
Bridges
Dentures (full and partial)
Implants (and implant-supported crowns/bridges, when the plan covers them)
Inlays/onlays (often treated as major restorative in many plans)
Periodontal surgery in some cases (gum surgery categories vary by plan)
Surgical/complex extractions in some plans (simple vs surgical can be classified differently)
You may see these services described under labels like major restorative, prosthodontics, endodontics, oral surgery, or periodontics. The section title changes, but the idea is the same: they’re not routine checkup-style services.
One practical note: some treatments are split across categories. Example: a root canal might be listed under a specialty category, while the crown that protects the tooth may be filed under major restorative. That’s why it helps to check each line item instead of assuming the “treatment plan” is one bucket.
Next, you’ll want to understand how plans separate preventive vs basic vs major, because that’s where confusion (and surprises) usually start.
Major vs Basic vs Preventive
Dental insurance usually sorts services into three buckets. The bucket matters because it determines which plan rules apply (how the service is processed, how strict the limits are, and what steps may be required).
Preventive = routine care that helps catch problems early and keep teeth stable.
Basic = simpler treatment to fix common issues once they show up.
Major = higher-complexity work that rebuilds, replaces, or restores function.
Preventive vs Basic vs Major Dental Care: Typical Examples
Category | Typical examples | Why plans group it here | What to confirm in your plan |
|---|---|---|---|
Preventive | Exams, cleanings, routine X-rays | Maintenance + early detection | How often it’s covered (frequency limits), whether you must use in-network providers |
Basic | Fillings, simple extractions, and gum treatment in some plans | Common repairs that are less complex than major rebuilds | Whether the plan labels these as “basic” or another category, and any limits or frequency rules |
Major | Crowns, bridges, dentures, and implants in some plans | Rebuild/replacement work that can involve more time, steps, or lab work | Whether each service is classified as major, whether pre-treatment estimates are recommended, and any exclusions or waiting periods |
Once you know which bucket your procedure sits in, you can predict the risk of surprise costs. Preventive and basic are usually simpler to process.
Major is where plan limits show up fast and where the math can change even when the procedure is “covered.” That’s the next piece to understand before you schedule anything.
Why Major Dental Care Creates Bigger Bills
Major dental care can still feel expensive even when you have coverage because “covered” does not mean “fully paid.” Major services are where plans tend to add the most rules, and those rules are what drive your out-of-pocket.
Here are the common reasons the bill jumps.

Annual maximums can cap what the plan pays.
Many dental plans have a yearly limit on how much they’ll pay toward your care. Major work can use up that limit quickly. Once you hit it, the rest of the cost can shift to you.
Waiting periods can delay help for major services.
Some plans don’t cover major services right away. They may require you to be enrolled for a set time before the plan pays toward crowns, bridges, dentures, or similar categories.
Timing and rules vary by plan, but the impact is the same: you may be paying more than you expected if you schedule too soon.
Limits and exclusions show up more often in “major.”
Major services are where plans commonly apply restrictions like frequency rules (how often something can be replaced), replacement rules (what qualifies for a new one), or specific exclusions tied to certain situations.
The plan may still cover the service category, but limit when it applies.
Network pricing changes the baseline cost.
Even before insurance pays anything, the “allowed amount” can differ depending on whether a dentist is in-network. In-network pricing is typically negotiated.
Out-of-network pricing can leave you exposed to a larger remaining balance, depending on how the plan calculates what it will pay.
This is where “paying cash by accident” happens.
A plan can show the service as “covered,” but apply rules that shift more of the cost to you than you anticipated. The practical fix is to verify the category and the plan rules before you commit to treatment.
What To Check Before Scheduling Major Dental Work
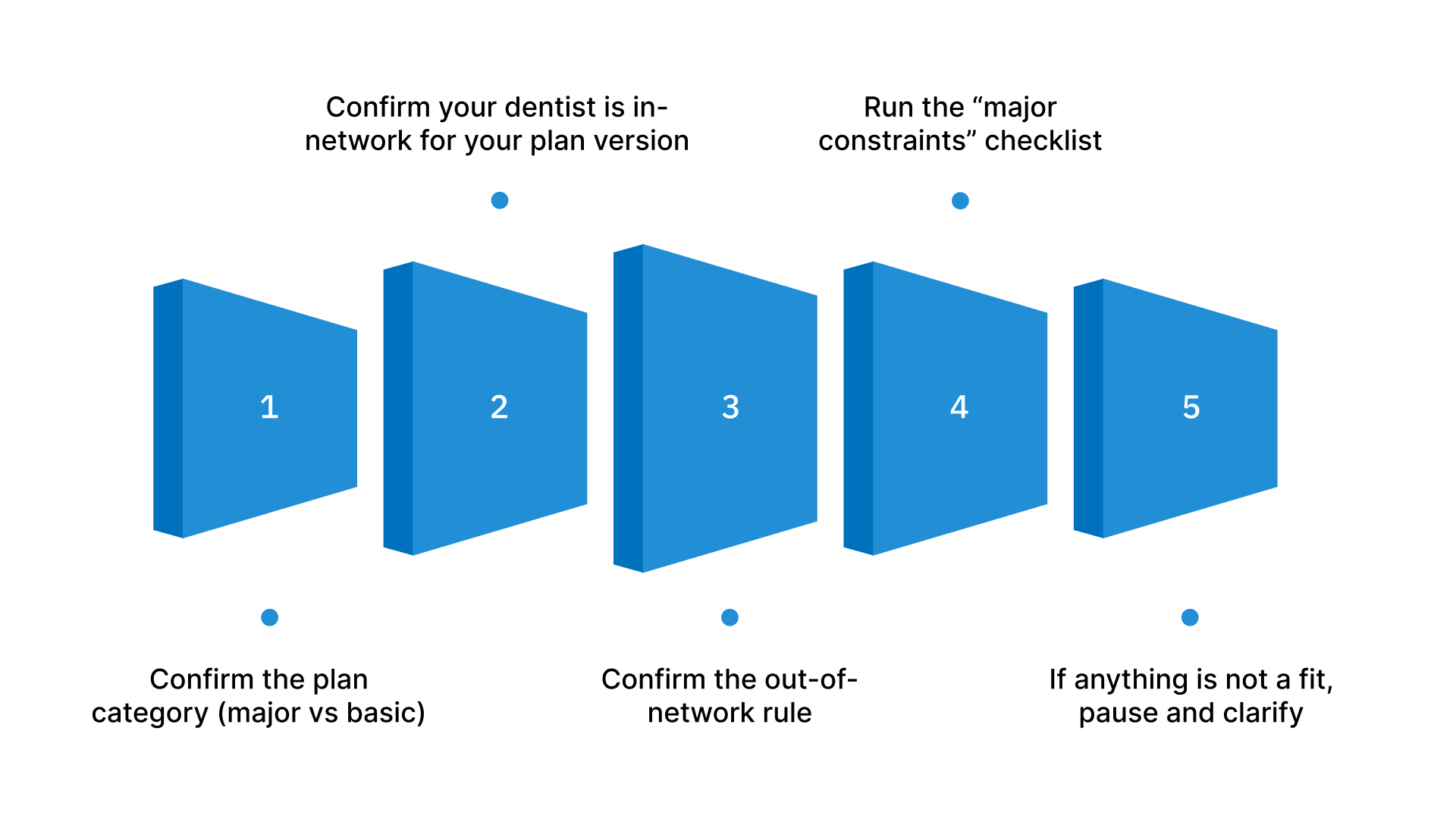
Major work is where small assumptions turn into big bills. Do this quick verification pass before you book.
Confirm the plan category (major vs basic).
Look in your plan summary for the service category your dentist mentioned. Don’t rely on what “usually” counts as major.
Confirm your dentist is in-network for your plan version.
Check the plan’s provider directory for your ZIP code. Search for the dentist by name + location. If the directory looks outdated, call the plan to confirm.
Confirm the out-of-network rule.
Is out-of-network covered, limited, or not covered for this plan? If it’s unclear, treat that as a stop sign until you get a clear answer.
Run the “major constraints” checklist.
You do not need to review the full policy. Just confirm whether any of these rules apply to this service:
Annual maximum
Waiting period
Replacement/frequency rule
Exclusions that could affect this case
If anything is not a fit, pause and clarify. Don’t guess.
Ask the plan or the office for the exact section in the plan summary that answers it.
If the work is expensive or the plan rules still feel unclear, a pre-treatment estimate is often the cleanest next step.
When a Pre-Treatment Estimate Is Worth Requesting
A pre-treatment estimate is a plan review of a proposed treatment plan before care is completed. It helps you understand how the plan is likely to process the service and whether any plan rules are likely to apply.
When is it worth requesting
Request one when:
The treatment is clearly in the major category or could be categorized in more than one way.
You are trying to keep costs predictable and need a clearer picture before scheduling.
The plan language is unclear, or the office is not confident about how the service will be processed.
Your dentist recommends multiple steps (for example, separate items on the treatment plan), and you want clarity on how each line will be handled.
What does it help you avoid?
A pre-treatment estimate does not eliminate all variables, but it can reduce avoidable surprises, such as:
A service being processed under a different category than expected.
Coverage being affected by plan limits that are easy to miss at a glance.
A mismatch between how the office described the plan and how the plan applies rules to the claim.
What the office usually needs
In most cases, the dental office can submit the request with:
Your plan details (member information or plan ID).
The provider’s details (dentist and location).
A short treatment plan summary (procedure codes and tooth number when relevant).
If the office will not submit it, ask them for the written treatment plan summary so you can request the estimate directly through the plan.
Once you have the estimated response, you can decide whether to proceed, adjust the plan, or confirm a better in-network option before committing to treatment.
TrueCost Group As The Next Step If Major Dental Costs Feel Out Of Reach
If you’re trying to plan for major dental work on a tight budget, the hardest part is not understanding the procedure. It’s choosing coverage without accidentally enrolling in a plan that does not work in your area or does not apply the way you expected.
TrueCost Group helps you understand dental plan options in plain language and enroll with advisor support. The goal is clarity. You get help sorting through plan terms, network rules, and real-world fit for your ZIP code.
Why this helps when money is tight:
It reduces guesswork when plan documents feel unclear or inconsistent.
It lowers the risk of enrolling based on assumptions that can lead to higher out-of-pocket costs later.
It saves time by narrowing options to what is more likely to fit your needs and timeline.
What to expect:
A clearer sense of which type of dental plan aligns with your situation.
Cleaner next steps for enrollment, without getting stuck in plan terminology.
Less time spent comparing random pages and more confidence in the decision you make.
If you want help reviewing dental plan options, reach out on Messenger for a free dental plan options check.
Before you choose, remember: the label matters less than what the plan actually does in your ZIP code.
Conclusion
“Major dental care” is a category label, not a fixed list. So the smartest move is to treat every treatment plan as a set of line items that must be matched to your benefits summary and network rules.
Before you commit to anything, confirm how the plan classifies the service, whether your dentist is contracted for your exact plan, and whether any timing or replacement limits apply. Those checks take minutes, but they prevent the most common coverage misunderstandings.
If you are still unsure after checking the basics, pause before scheduling. Getting clarity first is usually cheaper than correcting a plan decision later.
FAQs
What is considered major dental care?
Major dental care usually includes complex restorations or tooth replacement work, such as crowns, bridges, dentures, or implants. What counts as “major” is defined by the plan, so confirm the category in your plan summary.
Is a crown considered major dental care?
In many dental plans, yes, crowns are commonly listed under major services. Still, classification can differ by plan, so verify it in your Summary of Benefits. If the cost is high, a pre-treatment estimate can reduce uncertainty.
Is a root canal major dental care?
Not always. Some plans place root canals under basic services, while others categorize them differently. Check how your plan labels endodontic services before you schedule.
Do dental plans cover major dental work?
Many plans do, but coverage often comes with conditions. Waiting periods, annual maximums, and replacement or frequency limits can change your final out-of-pocket.
What’s the difference between basic and major dental care?
Basic care usually covers simpler repairs, while major care covers more complex rebuilds or replacements. The category matters because it affects plan rules, limits, and how the claim is handled.


