Introduction
Root canal treatment is a dental procedure that removes infected or damaged pulp from inside a tooth, cleaning and sealing it to save the natural tooth. If you've been told you need a root canal, are experiencing severe tooth pain, or simply want to understand the process before treatment, this guide walks you through every step.
Root canals have an intimidating reputation, but modern techniques and anesthesia make them comparable to getting a filling. In fact, over 15 million root canals are performed successfully in the United States each year, with patient-reported pain levels during treatment often similar to or lower than those experienced during standard dental fillings.
TL;DR
- Root canals remove infected pulp, clean the tooth, and seal it to prevent reinfection
- Most procedures take 60-90 minutes and can be completed in one or two appointments
- Modern anesthesia means little to no pain during treatment
- Recovery takes less than a week with mild sensitivity managed by over-the-counter pain relievers
- Success rates range from 86-97%, and treated teeth can last a lifetime with proper care
What Is Root Canal Treatment?
Root canal treatment (also known as endodontic therapy) treats infection or damage in the tooth's pulp—the soft tissue containing nerves, blood vessels, and connective tissue inside the tooth.
The goal is simple: Save your natural tooth by removing diseased pulp, eliminating infection, and preventing extraction.
How it differs from other procedures:
- vs. Tooth extraction: Saves the natural tooth rather than removing it
- vs. Standard filling: Treats deep pulp infection rather than surface cavities
Once a tooth is fully mature, it can survive without the pulp because it continues to be nourished by the tissues surrounding the root.
This makes root canal treatment a viable solution for preserving teeth that would otherwise require extraction.
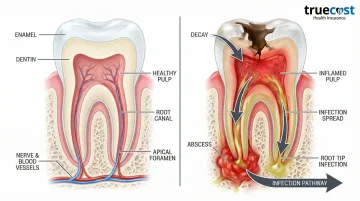
Why Root Canal Treatment Is Necessary
Common Causes
Root canal treatment becomes necessary when the pulp becomes infected or inflamed due to:
- Deep decay that reaches the pulp tissue
- Repeated dental procedures on the same tooth that stress the pulp
- Cracks or chips that expose the pulp, even without visible damage
- Dental abscesses from bacterial infection
- Trauma to the tooth from injury or impact
Risks of Leaving Infection Untreated
Ignoring an infected tooth leads to serious complications:
- Worsening pain that becomes unbearable
- Infection spread to surrounding bone and tissues
- Abscess formation with pus and swelling
- Bone loss around the root tips
- Tooth loss requiring extraction
- Systemic infection in rare cases, potentially spreading to other areas
Fortunately, modern treatment offers an effective solution to these risks.
High Success Rates
Root canal treatment is highly effective, with research showing success rates between 86% and 97% over 5 to 10 years. The procedure preserves your natural tooth while eliminating infection.
Endodontists (specialists in root canal treatment) achieve even higher success rates—98.1% compared to 89.7% for general dentists in complex cases.

The Root Canal Process: Diagnosis to Treatment
Initial Diagnosis and Consultation
Your dentist diagnoses the need for a root canal through several methods:
Diagnostic Tests:
- Clinical examination: Checking for pain, swelling, and tenderness
- X-rays: Visualizing infection or bone loss around the root
- Pulp vitality tests: Using cold or heat to assess nerve health
- Percussion tests: Tapping the tooth to determine if inflammation has spread to supporting bone
During the consultation, your dentist will:
- Discuss your symptoms and pain levels
- Review X-rays and test results
- Explain treatment options (root canal vs. extraction)
- Create a personalized treatment plan
- Answer questions about the procedure and recovery
Preparation for the Procedure
Before starting, your dentist ensures your comfort:
- Local anesthesia: Your dentist numbs the area completely—the same type used for fillings
- Rubber dam placement: Isolates the tooth and keeps it dry during treatment
- Comfort check: Ensures you feel no pain before proceeding
Once you're comfortable and numb, the procedure begins.
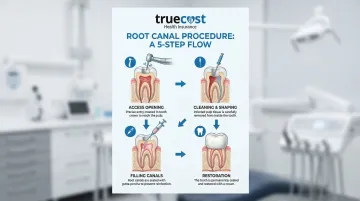
The Root Canal Procedure Steps
Step 1: Access Opening
The dentist creates a small opening in the tooth's crown to access the pulp chamber. This is similar to preparing a tooth for a filling and allows access to the infected area.
Step 2: Pulp Removal
Using specialized instruments called endodontic files, the dentist carefully removes the infected or damaged pulp from the pulp chamber and root canals.
This eliminates the source of infection and pain.
Step 3: Cleaning and Shaping
The dentist thoroughly cleans and shapes the inside of the root canals, removing all bacteria and debris.
The canals are irrigated with antimicrobial solutions (typically sodium hypochlorite) to disinfect the entire area.
Step 4: Filling the Canals
Once cleaned, the canals are filled with gutta-percha—a biocompatible, rubber-like material that has been the standard for over a century. Dental cement seals the filling to prevent future infection.
Step 5: Temporary or Permanent Restoration
A temporary filling may be placed if the tooth needs time to heal, or a permanent filling or crown may be placed in the same appointment depending on your case.
Multi-Appointment Treatment
Some cases require multiple visits:
Reasons for multiple appointments:
- Severe infection requiring drainage between visits
- Complex canal anatomy that takes longer to clean
- Dentist preference for a staged approach
Between appointments:
- A temporary filling protects the tooth
- Antibiotics may be prescribed to control infection
- Avoid chewing on the treated side
- Return for the second appointment as scheduled
Most procedures take 60-90 minutes per appointment. Single-visit treatments average 62 minutes, while multi-visit protocols average 93 minutes total chairside time.
Recovery and Post-Treatment Care
Immediate Post-Procedure (First 24 Hours)
- Numbness wears off within 2-4 hours
- Mild discomfort or sensitivity is normal as the area heals
- Avoid eating until numbness subsides to prevent biting your cheek or tongue
- Stick to soft foods initially to protect the temporary filling
First Week Recovery
Most people return to normal activities within 1-2 days:
- Mild soreness can be managed with over-the-counter pain relievers (ibuprofen 600-800mg or acetaminophen)
- Avoid chewing on the treated tooth until permanent restoration is complete
- Jaw soreness from keeping your mouth open during the procedure typically resolves in a few days
- Pain intensity drops significantly after the first 2 days
Follow-Up Restoration Appointment
You must return to have a permanent crown or filling placed to protect the treated tooth. This step is critical for long-term success.
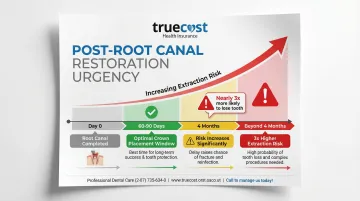
Timing matters:
- Schedule the permanent restoration within 60-90 days after the root canal
- Teeth receiving a crown more than 4 months after treatment are nearly 3 times more likely to be extracted
- Delays beyond 60 days significantly increase the risk of tooth loss
Long-Term Care
With proper care, a root canal-treated tooth can last a lifetime:
- Brush and floss regularly, treating it like any other tooth
- Attend routine dental checkups every 6 months
- Maintain good oral hygiene—the tooth can still develop decay or gum disease
When to Call Your Dentist
Contact your dentist immediately if you experience:
- Severe pain lasting more than a few days
- Visible swelling inside or outside the mouth
- Allergic reaction to prescribed medications
- Temporary filling coming loose or falling out
- Uneven bite when teeth come together
These symptoms may indicate complications requiring prompt attention.
Common Concerns and Misconceptions About Root Canals
Myth: Root Canals Are Extremely Painful
Reality: Modern anesthesia and techniques mean most patients feel little to no pain during the procedure. The pain people associate with root canals comes from the infection itself, not the treatment.
Pain levels during root canal therapy are comparable to getting a filling. For many Americans, fear of pain—combined with concerns about the cost of dental procedures—leads to delayed treatment, which only worsens the infection and discomfort.
Myth: Root Canals Cause Illness or Systemic Health Problems
Reality: Scientific research has thoroughly debunked this claim. The myth stems from the outdated "focal infection theory" from the 1920s. Root canals actually eliminate infection rather than cause it. The American Association of Endodontists states clearly that root canal treatment is safe and effective.
Myth: Root Canals Are Too Expensive to Afford
Reality: Many people avoid necessary dental care due to cost concerns, but options exist to make treatment accessible. Most dental insurance plans cover 50-80% of root canal costs, and many ACA marketplace health plans include pediatric dental coverage as an essential health benefit.
For adults, supplemental dental coverage through Medicare Advantage plans or standalone dental policies can significantly reduce out-of-pocket expenses. Payment plans and dental savings programs also help spread costs over time, making treatment more manageable than emergency care for untreated infections.
Normal vs. Abnormal Post-Treatment Symptoms
| Normal (Temporary & Expected) | Abnormal (Call Your Dentist) |
|---|---|
| Mild tenderness for a few days | Severe pain lasting more than a few days |
| Jaw soreness from keeping mouth open | Swelling that worsens or doesn't improve |
| Slight sensitivity when chewing | Fever or signs of allergic reaction |
| Persistent severe pain (rare, but requires immediate attention) |
Frequently Asked Questions
What is the step-by-step process of a root canal?
The dentist numbs the area, creates an opening in the tooth, removes infected pulp, cleans and disinfects the canals, fills them with gutta-percha, and seals with a restoration. This systematic process eliminates infection while preserving your natural tooth.
How long does a root canal take from start to finish?
The procedure typically takes 60-90 minutes, though complex cases may take longer. The complete process including the follow-up restoration appointment takes 2-4 weeks from initial treatment to final crown placement.
Can a root canal cause ear pain?
Temporary ear pain or jaw soreness is possible due to referred pain from inflammation and keeping your mouth open during the procedure. This should resolve within a few days, as the ear and teeth share nerve pathways.
Does a root canal hurt?
Modern anesthesia makes root canals no more painful than getting a filling. Mild post-procedure soreness is normal and manageable with over-the-counter pain relievers. The treatment actually relieves the severe pain caused by the infection, not creates it.
How much does a root canal cost?
Root canal costs typically range from $620 to $1,500 depending on tooth location and complexity. Front teeth cost $620-$1,100, premolars run $720-$1,300, and molars range from $890-$1,500. Dental insurance often covers 50-80% of the procedure after deductibles.
TrueCost Group's licensed advisors can help you find health insurance plans with dental benefits. Many Medicare Advantage plans include coverage for major procedures. Call 1-888-788-8285 to explore your options.
What can I eat after a root canal?
Stick to soft foods for the first few days: yogurt, smoothies, mashed potatoes, scrambled eggs, soft pasta, and lukewarm soups. Avoid hard, crunchy, or chewy foods that could damage the temporary filling, and chew on the opposite side until the permanent restoration is complete.