Introduction: Don't Ignore These Warning Signs
You've been putting off that dental visit for weeks. The tooth pain comes and goes, and you tell yourself it's just sensitivity.
But that constant ache when you bite down isn't going away—and it's trying to tell you something important.
Recognizing the early warning signs of needing a root canal can mean the difference between saving your tooth and losing it entirely. More than 15 million teeth are saved each year through root canal treatment, yet many people delay care until the infection spreads beyond the tooth.
This guide covers the specific symptoms that signal you need a root canal, the risks of delaying treatment, what the procedure involves, and how ACA marketplace and Medicare Advantage plans make root canals affordable—even if you're currently uninsured.
TLDR:
- Sensitivity to hot/cold lasting 30+ seconds signals nerve damage needing immediate treatment
- Untreated infections spread to your jawbone and bloodstream, risking hospitalization
- Modern root canals are comfortable procedures that relieve pain rather than cause it
- Saving your tooth with a root canal costs less long-term than extraction and implant replacement
- 80% of Americans qualify for $0-$50/month health plans that include dental coverage for major procedures like root canals
Warning Signs You Need a Root Canal
Persistent, Severe Tooth Pain
The most common indicator of needing a root canal is tooth pain that won't quit. But not all tooth pain signals a root canal.
The key distinction is persistence. If discomfort lasts for days rather than fleeting moments, your tooth pulp may be irreversibly damaged.
Pain when chewing or applying pressure to the tooth suggests inflammation has spread to the periodontal ligament (tissue surrounding) the root. This isn't the brief sensitivity you might feel with a cavity. Instead, it's a deep, throbbing ache that interferes with eating and sleeping.
Prolonged Sensitivity to Temperature
Another telltale sign involves how your tooth reacts to hot and cold. Here's the critical diagnostic threshold: sensitivity that lingers 30 seconds or longer after removing a hot or cold stimulus indicates irreversible pulpitis (inflamed pulp that cannot heal on its own).
The difference matters:
- Reversible sensitivity: Pain disappears within seconds after removing ice water or hot coffee (typically means you need a filling)
- Irreversible damage: Discomfort continues for 30+ seconds after the temperature source is gone (signals you need a root canal)
This prolonged reaction indicates the nerve inside your tooth is damaged beyond the point of self-healing.
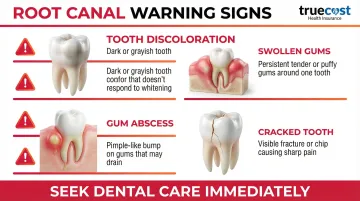
Visible Warning Signs
Your tooth and surrounding gums may show physical symptoms:
- Tooth discoloration: Darkening or grayish appearance indicates pulp necrosis (tissue death)
- Swollen or tender gums: Inflammation near the affected tooth, often sensitive to touch
- Pimple-like bump on gums: Called a dental abscess or sinus tract, this may drain pus and indicates active infection
- Cracked or chipped teeth: Even without immediate pain, damage that exposes the inner pulp creates a pathway for bacteria
The Silent Threat: No Symptoms
Sometimes there are no symptoms initially. The infection develops quietly, only detectable through X-rays during routine dental exams. This is why regular checkups (every six months) are critical—they catch problems before they cause pain or require emergency treatment.
Assessing Urgency: When to Call Immediately
Seek emergency dental care if you experience:
- Fever accompanying tooth pain
- Facial swelling or difficulty swallowing
- Severe, unbearable pain that doesn't respond to over-the-counter medication
- Difficulty opening your mouth (trismus)
Schedule an appointment within 1-2 weeks for:
- Mild but persistent discomfort lasting several days
- Lingering sensitivity to temperature
- Visible gum swelling or discoloration
What Causes the Need for a Root Canal?
Three Primary Causes
Your tooth's pulp—the soft tissue inside containing nerves and blood vessels—becomes infected or inflamed through specific pathways:
Deep tooth decay: The most common and preventable cause. Bacteria from untreated cavities penetrate through enamel and dentin layers to reach the pulp chamber.
Trauma or injury: A blow to the tooth from sports injuries or accidents can damage the pulp even without visible cracks. The impact may sever the blood supply, causing tissue death over time.
Repeated dental procedures: Multiple treatments on the same tooth create cumulative stress and inflammation to the pulp, eventually causing irreversible damage.
How Bacteria Invade the Tooth
Once bacteria enter the pulp chamber through cracks, chips, or deep cavities, the tissue becomes inflamed. Because the pulp is encased in hard dentin, inflammation increases pressure inside the tooth, cutting off blood flow.
Without blood supply, the tissue dies (necrosis). Dead pulp tissue then becomes a breeding ground for bacteria.
The infection follows a destructive path:
- Bacteria multiply inside the dead pulp tissue
- Infection exits through the root tip into surrounding jawbone
- An abscess forms, destroying bone tissue around the root
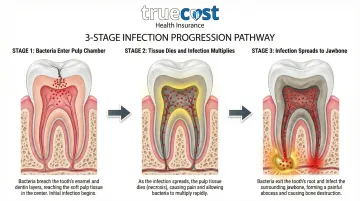
The Most Preventable Cause
Understanding how infections spread makes prevention clear: untreated cavities account for the majority of root canal cases. Small cavities that could be fixed with simple fillings progress into deep decay requiring root canal treatment when ignored.
This progression is entirely preventable through regular dental visits and addressing problems early.
What Happens If You Delay Root Canal Treatment
Infection Spreads Beyond the Tooth
Dental infections don't resolve on their own. Without treatment, bacteria multiply and spread through the root canals into the alveolar bone (jawbone), causing an acute apical abscess.
This infection destroys the bone surrounding the tooth root, creating a pocket of pus that causes intense pain and swelling. In severe cases, the infection spreads to the fascial spaces of the neck or enters the bloodstream, potentially causing sepsis—a life-threatening condition requiring hospitalization and intravenous antibiotics.
Hospitalization Risks Are Real
Dental infections drive thousands of emergency department visits annually:
- Approximately 5% of patients presenting to the ED with dental complaints require hospital admission
- Of those admitted, 85% have infections involving the pulp or tissues surrounding the tooth root
- Complications like deep neck space infections or airway compromise require urgent hospitalization
These aren't just statistics—they represent preventable medical emergencies that started as treatable tooth infections. For individuals without dental coverage, these emergency visits can result in thousands of dollars in hospital bills. Many comprehensive health insurance plans cover emergency medical treatment for dental infections, though routine dental procedures may require separate coverage.
Bone Loss Makes Teeth Unsalvageable
Chronic infection causes progressive destruction of the bone anchoring your tooth. Once bone loss becomes extensive, the tooth cannot be saved—even with a root canal. At that point, extraction becomes the only option.
This is the "point of no return": waiting too long eliminates your chance to save the natural tooth, forcing you into more expensive tooth replacement options like implants or bridges.
The Progression Timeline
Here's how quickly a treatable infection becomes a costly emergency:
Week 1-2: Infection confined to the tooth pulp—treatable with standard root canal Week 3-4: Infection spreads to surrounding bone—still treatable but with more extensive procedures Month 2-3: Significant bone loss occurs—tooth may become unsalvageable Month 3+: Extraction required, followed by bone grafting and implant placement costing $3,000-$6,000

What could have been resolved with a $1,000-$1,500 root canal becomes a $5,000+ reconstruction.
When Pain Disappears, the Problem Hasn't
Many people believe that if tooth pain suddenly stops, the problem has resolved. This is dangerously false. Pain disappearing often means the nerve has died—but the infection remains active and continues spreading through the bone. You've lost the warning signal while the disease progresses silently.
Understanding Root Canal Treatment: What to Expect
Dispelling the Pain Myth
Modern root canal treatment is not painful. This outdated reputation comes from the era before advanced anesthesia. Today's local anesthetics make the procedure comfortable—most patients report feeling pressure but no pain during treatment.
The reality: root canals relieve pain rather than cause it. The severe discomfort you're experiencing comes from the infected pulp. Removing that infection eliminates the source of pain.
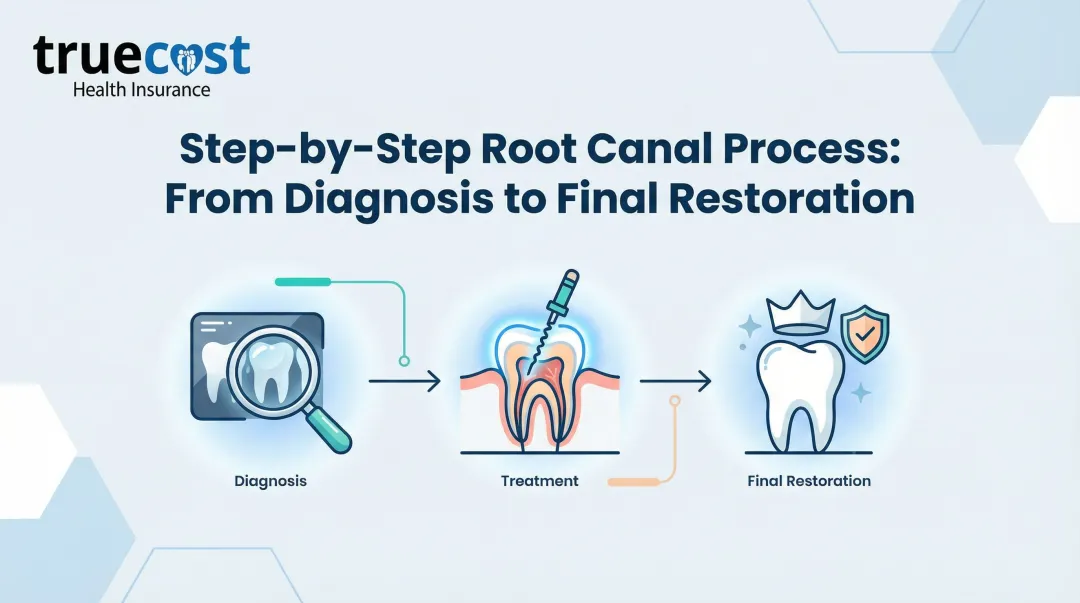
The Procedure: Step-by-Step
1. Numbing and isolation (10-15 minutes): Your endodontist gives local anesthesia to completely numb the tooth. A dental dam (protective rubber sheet) isolates the tooth, keeping it clean and dry during treatment.
2. Access and cleaning (30-45 minutes): The endodontist makes a small opening in the tooth's crown. Specialized instruments remove the infected pulp from the pulp chamber and root canals. The canals are cleaned with sodium hypochlorite solution to eliminate bacteria.
3. Shaping and filling (20-30 minutes): The cleaned canals are shaped to receive filling material. Gutta-percha (a biocompatible rubber-like material) fills the canals, sealed with adhesive cement to prevent future infection.
4. Temporary restoration (5-10 minutes): A temporary filling seals the access opening until you return to your general dentist for the permanent crown.
Timeline and Appointments
Understanding the time commitment helps you plan around work and other obligations:
- Most root canals: Completed in 1-2 appointments
- Appointment length: 60-90 minutes each
- Tooth type matters: Front teeth (one canal) typically require one visit; molars (3-4 canals) may need two visits
Recovery Expectations
Immediately after treatment:
- Numbness wears off within 2-3 hours
- Mild soreness or sensitivity for 2-3 days
- Pain manageable with ibuprofen or acetaminophen
Activity and diet:
- Return to work or normal activities the same day
- Avoid chewing on the treated tooth until the permanent crown is placed
- No dietary restrictions beyond avoiding hard foods on that side
The Critical Final Step: Crown Placement
After root canal treatment, the tooth needs a permanent crown for protection. Root canal-treated teeth become more brittle because they no longer have blood supply.
Why the crown matters:
- Prevents the tooth from cracking or breaking during normal chewing
- Typically placed by your general dentist 2-4 weeks after the root canal
- Without this final restoration, the tooth remains vulnerable to fracture
Skipping the crown can lead to tooth fracture—potentially requiring extraction despite the successful root canal.
Root Canal vs. Tooth Extraction: Making the Right Choice
When you have an infected tooth, you face a choice: save it with a root canal or remove it with extraction. The decision affects your oral health and wallet for years to come.
Comparing Success Rates
Both options have high success rates, but preserving your natural tooth offers distinct advantages:
| Treatment | Success Rate | Long-Term Outcome |
|---|---|---|
| Root Canal | 97% survival at 8 years | Natural tooth preserved, maintains bone |
| Dental Implant | 95% survival | Requires surgery, 3-6 month healing time |
| Bridge | 82% survival | Requires grinding down adjacent healthy teeth |
Beyond clinical success rates, the financial difference between these options is substantial.
The True Cost Comparison
Root canal + crown: $1,700-$4,000 total
- Root canal procedure: $700-$1,600
- Crown: $1,000-$2,500
Extraction + implant: $3,000-$6,000+ total
- Extraction: $200-$600
- Bone graft (often needed): $300-$1,200
- Implant placement: $1,500-$3,000
- Implant crown: $1,000-$2,000
Saving your natural tooth costs significantly less than replacing it.

Advantages of Preserving Your Natural Tooth
Choosing to save your natural tooth provides benefits that extend beyond initial cost savings:
- Your natural tooth root stimulates the jawbone during chewing, preserving bone density and strength
- Adjacent teeth stay in position after a root canal, preventing the drift and bite problems that occur when teeth are extracted
- The tooth root maintains bone volume, while extraction causes the bone to resorb (shrink away) by 25% in the first year alone
- Treatment completes in 3-4 weeks for root canal and crown versus 4-6 months for implant placement and healing
- Research shows natural teeth provide better long-term oral health outcomes than any replacement option
Cost of Root Canal Treatment and Insurance Options
Realistic Cost Ranges
Root canal costs vary based on the affected tooth and your geographic location:
| Tooth Type | Root Canal Cost | Crown Cost | Total Investment |
|---|---|---|---|
| Front Tooth | $700-$1,000 | $1,000-$1,500 | $1,700-$2,500 |
| Premolar | $800-$1,200 | $1,000-$2,000 | $1,800-$3,200 |
| Molar | $1,200-$1,800 | $1,000-$3,000 | $2,200-$4,800 |
These ranges reflect national averages. Costs in major metropolitan areas may run 20-30% higher, while rural areas may be 10-20% lower.
Dental Insurance Coverage
Most dental insurance plans categorize root canals as "major services" with specific coverage levels:
Typical coverage: Plans cover 50-80% of the procedure cost after your deductible. Most plans cap annual benefits at $1,000-$2,000, and some require 6-12 months enrollment before covering major procedures.
Before scheduling treatment:
- Verify your plan's coverage percentage for endodontics
- Confirm your remaining annual maximum
- Ask your dentist's office for a pre-treatment estimate showing your out-of-pocket cost
ACA Marketplace Plans with Dental Coverage
Beyond traditional dental insurance, you may have other options for covering major procedures.
Adult dental coverage is optional under the Affordable Care Act, so understanding your options matters:
Embedded dental plans: Only about 9% of ACA marketplace medical plans include built-in adult dental benefits.
These plans may cover major procedures like root canals, but often subject them to the medical deductible (averaging $3,000+).
Standalone dental plans: Available separately from medical coverage, these typically have lower deductibles ($50 average) with separate premiums. They generally cover 50% of major procedures after a waiting period.
Coverage availability varies significantly by state and carrier.
If you're exploring ACA marketplace options that include dental benefits for major procedures like root canals, TrueCost Group can help you identify plans that fit your needs. Our licensed insurance agents work with major carriers to find coverage options—call 1-888-788-8285 for personalized assistance.
Medicare Advantage Dental Benefits
Original Medicare does not cover routine dental care, including root canals, fillings, or extractions.
Medicare Advantage plans offer a different landscape:
- 97% of Medicare Advantage plans now include some dental benefits
- 84% offer comprehensive coverage that includes major procedures like root canals
- Annual caps apply: Most plans limit dental benefits to $1,000-$2,000 per year
Since a root canal and crown can easily exceed $2,000, you may still face significant out-of-pocket costs. Review your specific plan's dental benefit details to understand your coverage limits.
Frequently Asked Questions
How do I know if I need a root canal or just a filling?
Fillings treat decay in the outer tooth layers, while root canals address infection that's reached the inner pulp and nerve. Your dentist uses X-rays and sensitivity tests to determine which you need—only a professional exam can make the diagnosis.
Can a tooth infection spread to other parts of my body?
Yes. Untreated infections can spread to the jawbone, bloodstream, and surrounding tissues, potentially causing sepsis or deep neck infections that compromise breathing. Prompt treatment is critical—dental infections never resolve on their own.
How long can I wait to get a root canal?
Schedule treatment within 1-2 weeks of your dentist's recommendation. Waiting months increases your risk of bone loss, abscess formation, and tooth loss—the infection continues spreading and may make the tooth unsalvageable.
What happens if I can't afford a root canal?
ACA marketplace and Medicare Advantage plans often include dental coverage for major procedures. Dental schools, payment plans, and Federally Qualified Health Centers offer additional affordable options. Call TrueCost Group at 1-888-788-8285 to explore insurance plans with dental benefits.
Is it better to get a root canal or extract the tooth?
Saving your natural tooth with a root canal is preferable to extraction. Root canals cost less long-term ($1,700-$4,000 versus $3,000-$6,000 for extraction plus implant), maintain jawbone density, and prevent adjacent teeth from shifting.
Will I need to take time off work for a root canal?
Most people return to work the same day or next day. The 60-90 minute procedure causes only mild discomfort manageable with ibuprofen, and you can resume normal activities immediately.