
You might feel frustrated when you receive a surprise bill after thinking your insurance would cover a dental visit. Many people struggle to understand why a treatment was rejected or why the final cost remains so high.
It is common to feel confused by the complex language used in official documents sent by insurance providers. Understanding the process helps you ensure your dentist submits the right details to get your dental work covered.
This knowledge protects your household budget from unexpected expenses while helping you use your full benefits.
In this guide, you will learn how dental insurance claims function and how to manage them for your family.
Quick Look
Provider Responsibility: In-network dentists usually handle all the paperwork and submit claims directly to the insurer on your behalf.
Coding Accuracy: Every procedure uses a specific code that tells the insurance company exactly what work was performed today.
Financial Breakdown: The claim determines the specific portion you owe after deductibles and coinsurance percentages are applied correctly.
Review Process: Insurers check your eligibility and plan limits before they issue any payment to the dental office.
Evidence Requirements: Some major dental procedures require X-rays or clinical notes to prove the treatment was medically necessary.
What Are Dental Insurance Claims?
A dental claim is a formal request for payment sent to your insurance company after you receive dental care. It serves as an itemized bill that describes your treatments so the insurer can calculate your specific coverage benefits.
This document connects your dentist, your insurance policy, and your final payment to ensure everyone is billed accurately.
Why Dental Insurance Claims Matter
Understanding the claim process is essential because it directly impacts how much money stays in your own bank account. A correctly filed claim ensures you receive the highest level of coverage allowed under your current dental insurance policy.
You can avoid many common billing errors by knowing what information the insurance company needs to process your request:
Cost Determination: The claim defines the exact dollar amount the insurance company will pay toward your professional dental services.
Error Prevention: Checking your claims helps you spot mistakes that could lead to you paying much more than necessary.
Surprise Prevention: Familiarity with the process ensures you know exactly when and why you might receive a secondary bill.
Do you worry that one claim mistake could turn free cleanings or covered fillings into a costly bill? TrueCost Group helps you enroll in PPO dental plans where preventive exams, cleanings, and X-rays are covered, and claims are simpler. Get a free quote over text to see plans with no waiting periods, national PPO access, and up to $5,000 in annual coverage.
Knowing why these documents matter helps you stay organized as you move through the standard dental treatment process.
How Dental Insurance Claims Work
The lifecycle of a claim begins the moment you sit in the dental chair and ends with final payment. This process involves several checkpoints where information is verified to ensure that the treatment matches your specific plan rules.
You can follow these five steps to understand exactly what happens to your information after you leave the office:
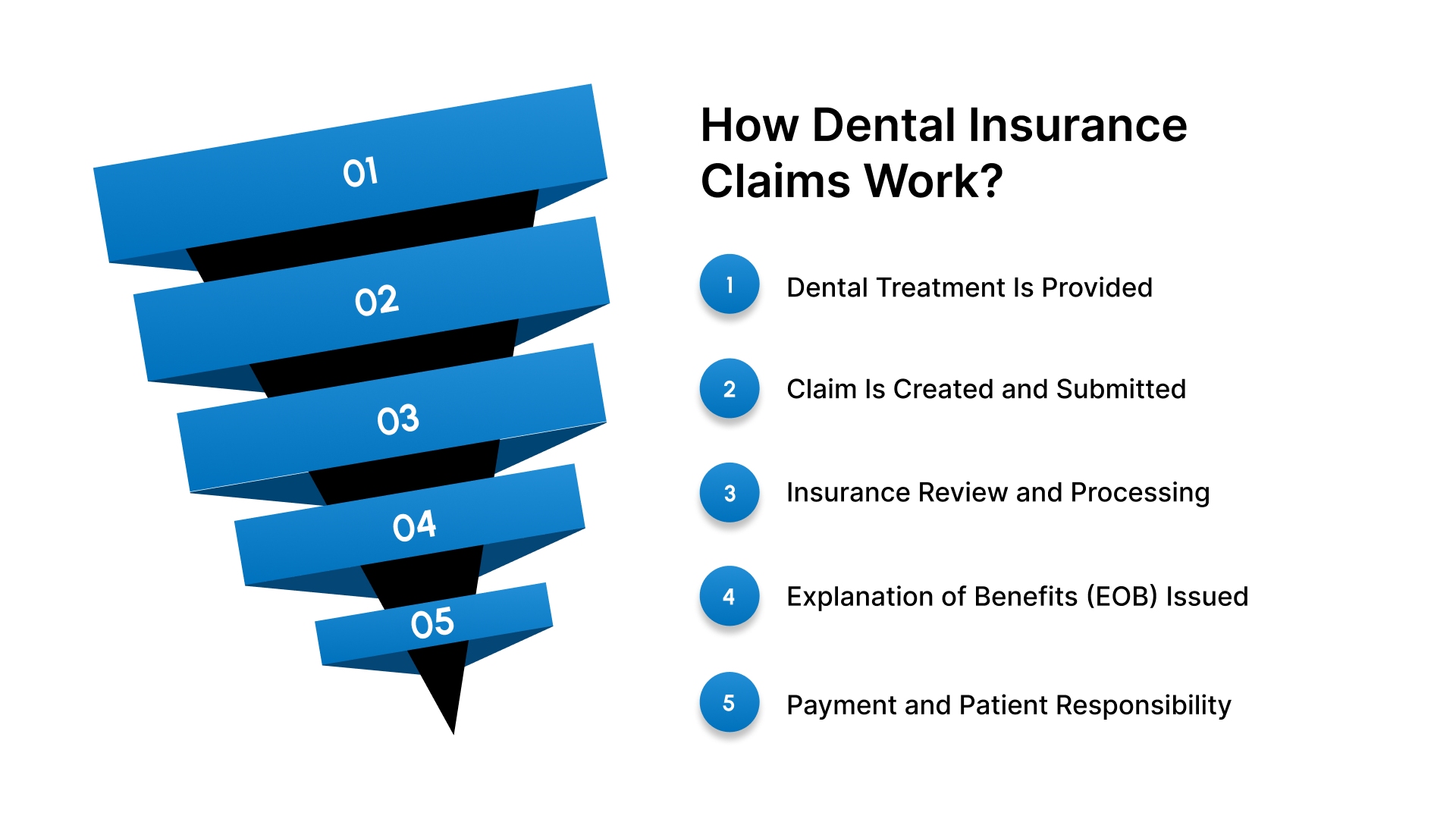
Step 1 – Dental Treatment Is Provided
Your dentist performs the necessary work and records the specific details of your visit in your medical file.
Staff members assign specific procedure codes to each task to describe the treatment to the insurance company later.
Choosing an in-network provider ensures that the office already understands the specific billing requirements for your dental plan.
Step 2 – Claim Is Created and Submitted
The dental office creates an official claim form that includes your member ID and the provider tax information.
Every service is listed with a corresponding CDT code which is a standard identifier for every dental procedure.
Most modern dental offices submit these claims electronically to speed up the review and payment process for patients.
Step 3 – Insurance Review and Processing
The insurance company verifies that your policy was active on the date the dental services were actually performed.
They apply your annual deductible and check if you have reached your annual maximum benefit for the year.
Typical processing times vary depending on whether the insurer needs extra information, like X-rays or a doctor’s note.
Step 4 – Explanation of Benefits (EOB) Issued
An EOB is a document that shows what the dentist billed and what the insurance company agreed to pay.
You should read each line to see the discounts applied and the amount the insurance company sent to the dentist.
This document is not a bill but a summary that helps you track your remaining benefits for the year.
Step 5 – Payment and Patient Responsibility
The insurance company sends a payment directly to the dentist for the portion covered under your specific plan.
You are responsible for paying any remaining balance, which often includes your coinsurance or your annual plan deductible.
You may receive a final invoice from the dentist after they receive the official payment from the insurance company.
Understanding this technical process makes it much easier to identify who is responsible for filing your paperwork each time.
Who Files Dental Insurance Claims?
Dental insurance claims are filed either by your dentist or by you, depending on the provider network status.
Knowing responsibility prevents missed deadlines and unpaid reimbursements:
When the Dentist Files the Claim
In-network providers have a legal agreement with the insurance company to handle all claim submissions for their covered patients. This arrangement is highly advantageous because it removes the burden of paperwork from you and reduces your immediate stress.
You usually only pay your estimated portion at the time of service, while the office waits for the insurance.
When You Must File the Claim Yourself
You might have to file a claim yourself if you visit an out-of-network dentist who does not accept assignment. This process requires you to pay the full bill upfront and then wait for the insurance company to reimburse you.
You must submit all required documentation and receipts before the established deadline to receive your money back from them.
If you find yourself in a situation where you must file alone, following a structured guide is very important.
How to File a Dental Insurance Claim Yourself
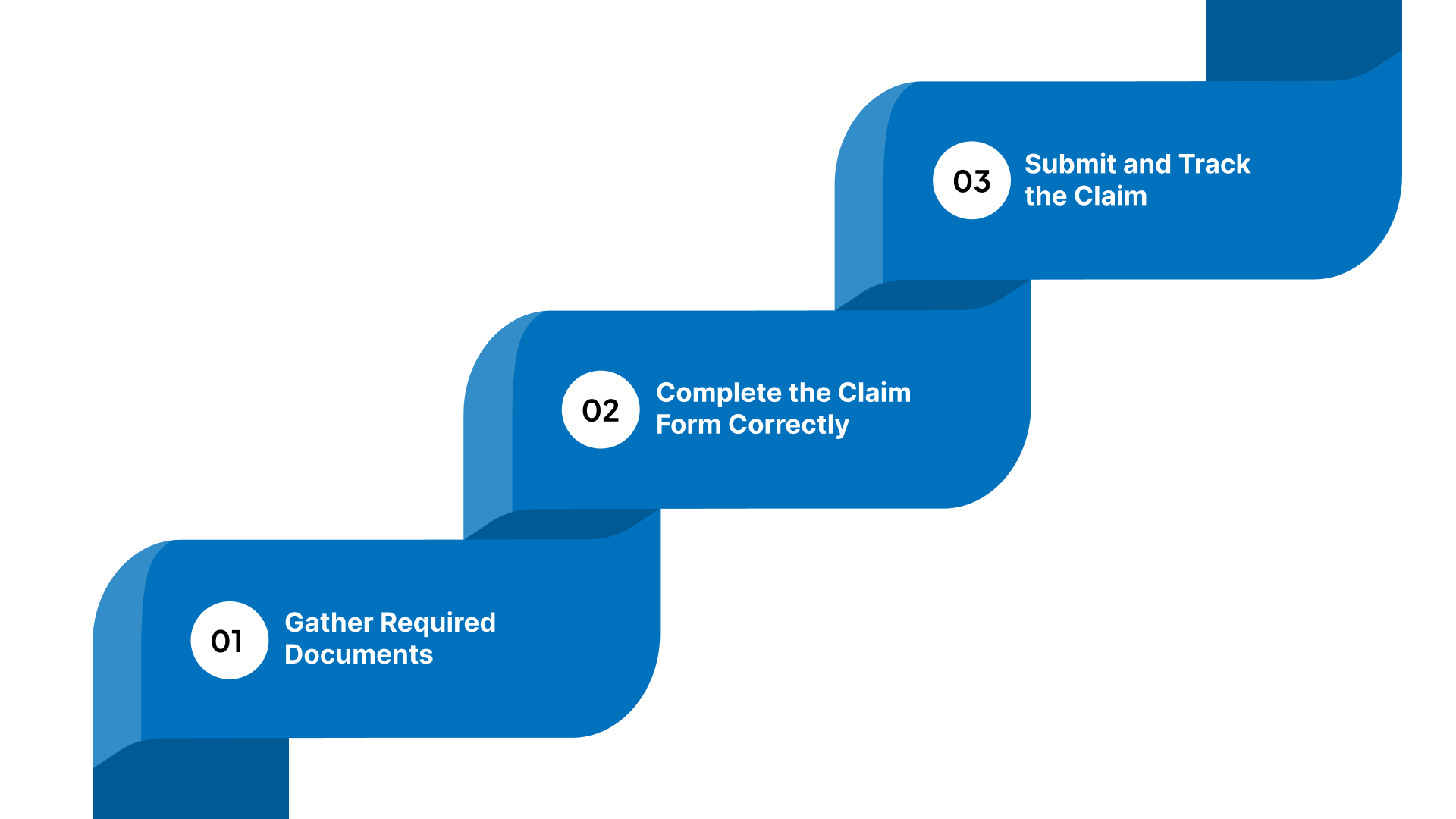
Filing your own claim is manageable if you gather all the necessary details before you start the official submission. You should be diligent about accuracy to ensure the insurance company does not reject your request due to small errors:
Step 1 – Gather Required Documents
Request a fully itemized receipt from your dentist that shows every procedure performed and the total cost paid.
Ensure the document includes the specific treatment codes and the exact date each service was completed in the office.
Write down the dentist's name, their office address, and their professional National Provider Identifier for the claim form.
Step 2 – Complete the Claim Form Correctly
Visit your insurance provider's website to download the most recent version of their official dental claim submission form.
Fill out every section clearly and double-check your member ID number to prevent any delays in the system.
Avoid leaving any fields blank because missing information is the most common reason for a claim to be rejected.
Step 3 – Submit and Track the Claim
Send your completed form and receipts through the insurer's online portal or by certified mail for a paper record.
Log in to your member account regularly to monitor the status of your claim as it moves through review.
Expect a response within thirty days, although some electronic submissions may be processed much faster than a paper form.
Understanding how to file a claim correctly helps you better predict how the insurance company calculates your final costs.
How Dental Insurance Claim Payments Are Calculated
Insurance companies calculate dental claim payments using plan-specific rules tied to negotiated rates and coverage limits. Dentists may bill higher amounts, but insurers pay only the allowed amount, which in-network providers accept fully.
You pay a deductible first, then share costs through coinsurance percentages. Annual maximums cap how much insurance pays yearly, so timing major treatments carefully helps you reduce total out-of-pocket dental expenses.
Understanding these calculations will help you spot the reasons why an insurance company might deny a specific dental claim.
Common Dental Insurance Claim Denials
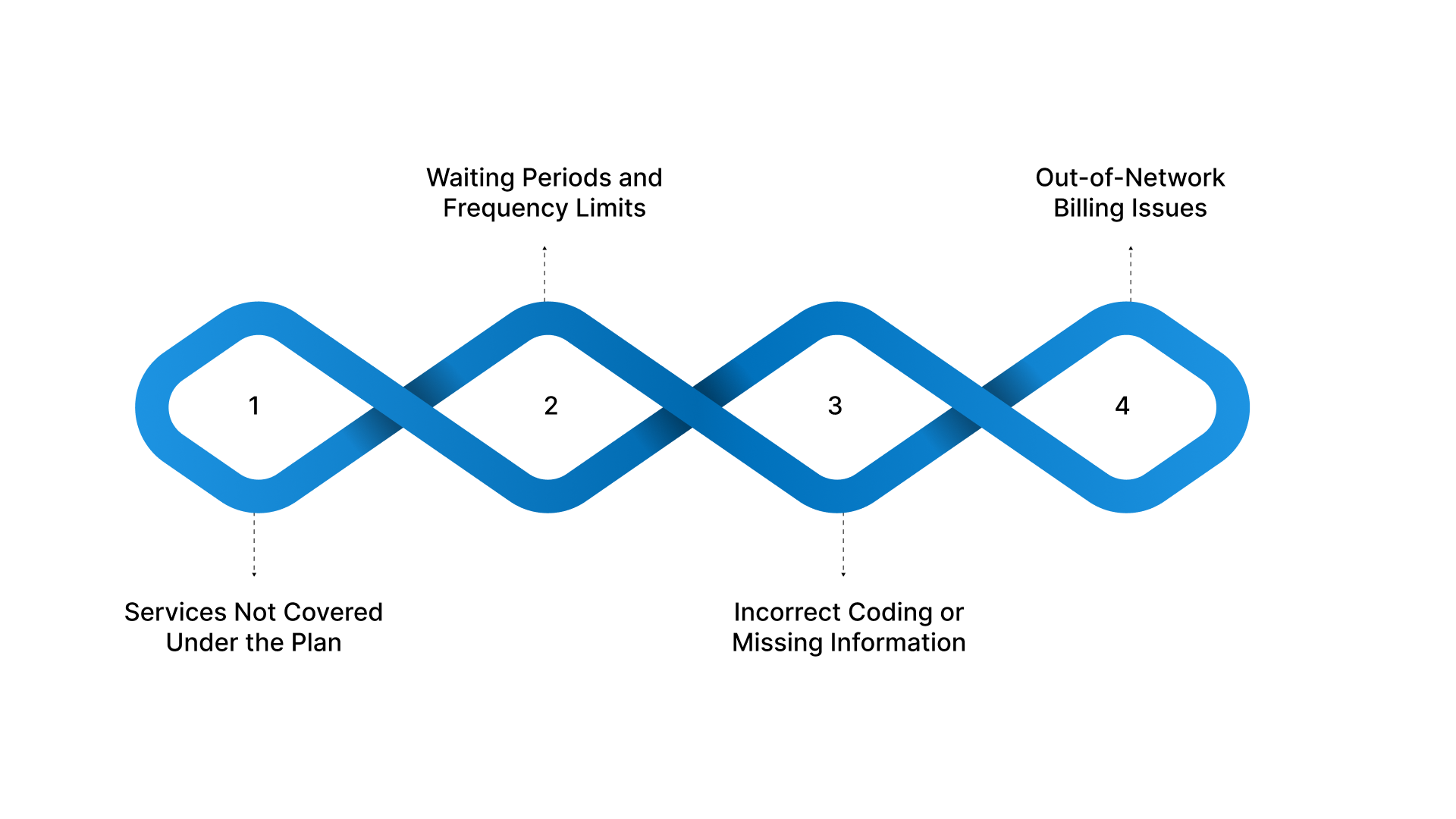
Claim denials can be frustrating, but most of them can be resolved by providing more information or correcting small errors. In fact, 15% of dental insurance claims were denied in 2025, often due to incorrect or missing information.
You should review every denial notice carefully to understand the specific reason why the insurance company refused the payment:
Services Not Covered Under the Plan
Some plans exclude specific treatments like teeth whitening or adult braces because they are considered cosmetic rather than necessary. You can fix this by asking your dentist to submit a pre-treatment estimate to verify coverage before the work begins.
Waiting Periods and Frequency Limits
Insurers often deny claims if you receive major work before your waiting period ends or if you exceed visit limits. You should check your plan details to ensure you have waited long enough before scheduling crowns or other major services.
Incorrect Coding or Missing Information
A simple typo in a procedure code or a missing tooth number can trigger an automatic denial from the insurer. You can fix this by asking the dental office to correct the error and resubmit the claim with clarity.
Out-of-Network Billing Issues
Claims might be denied or paid at a lower rate if you visit a dentist who is not in the network. You can reduce your responsibility by confirming your dentist's network status before every appointment to ensure you get discounts.
Finding coverage that minimizes these hurdles is often the best way to help you estimate how long your specific claim might take to finish.
How Long Do Dental Insurance Claims Take to Process?
The timeline for a claim depends on the method of submission and the complexity of the dental work performed. Most insurance companies aim to process requests as quickly as possible to maintain a positive relationship with their dental providers:
Typical Processing Timelines
Electronic claims usually take between seven and fourteen days to process, while paper claims can take up to thirty days. You will receive an EOB once the review is complete, which explains the final decision made by the insurance company.
Reasons Claims Take Longer Than Expected
Claims might slow down if the insurer requires more documentation, like a narrative from the dentist or older X-rays. Coordination of benefits can also add time if you have more than one insurance plan covering your dental work today.
Checking your status regularly can help you catch these delays before they become a major problem for your budget.
How to Check the Status of a Dental Insurance Claim
You do not have to wait for the mail to find out if your dental insurance claim was approved. Most modern insurance providers offer several ways to track your request in real-time through their own digital customer service tools:
Checking Through Insurance Portals
You can log in to your secure member portal to see a list of all recent claims and their status. These portals explain whether a claim is currently pending, approved for payment, or denied by the insurance review team.
Contacting the Dentist or Insurer
You can call the dental office billing coordinator to ask if they have received a response from the insurance company. If the claim is taking too long, calling the insurer directly can help you identify if any information is missing.
Are you tired of tracking claims and still wondering if crowns, root canals, or extractions will be covered? TrueCost Group helps you choose PPO dental plans designed to reduce claim confusion with in-network dentists. Get a free quote over text to review month-to-month plans that include fillings, major procedures and more.
Taking these proactive steps will ensure that your claims move through the system without any unnecessary or stressful delays.
Best Practices to Avoid Dental Insurance Claim Problems
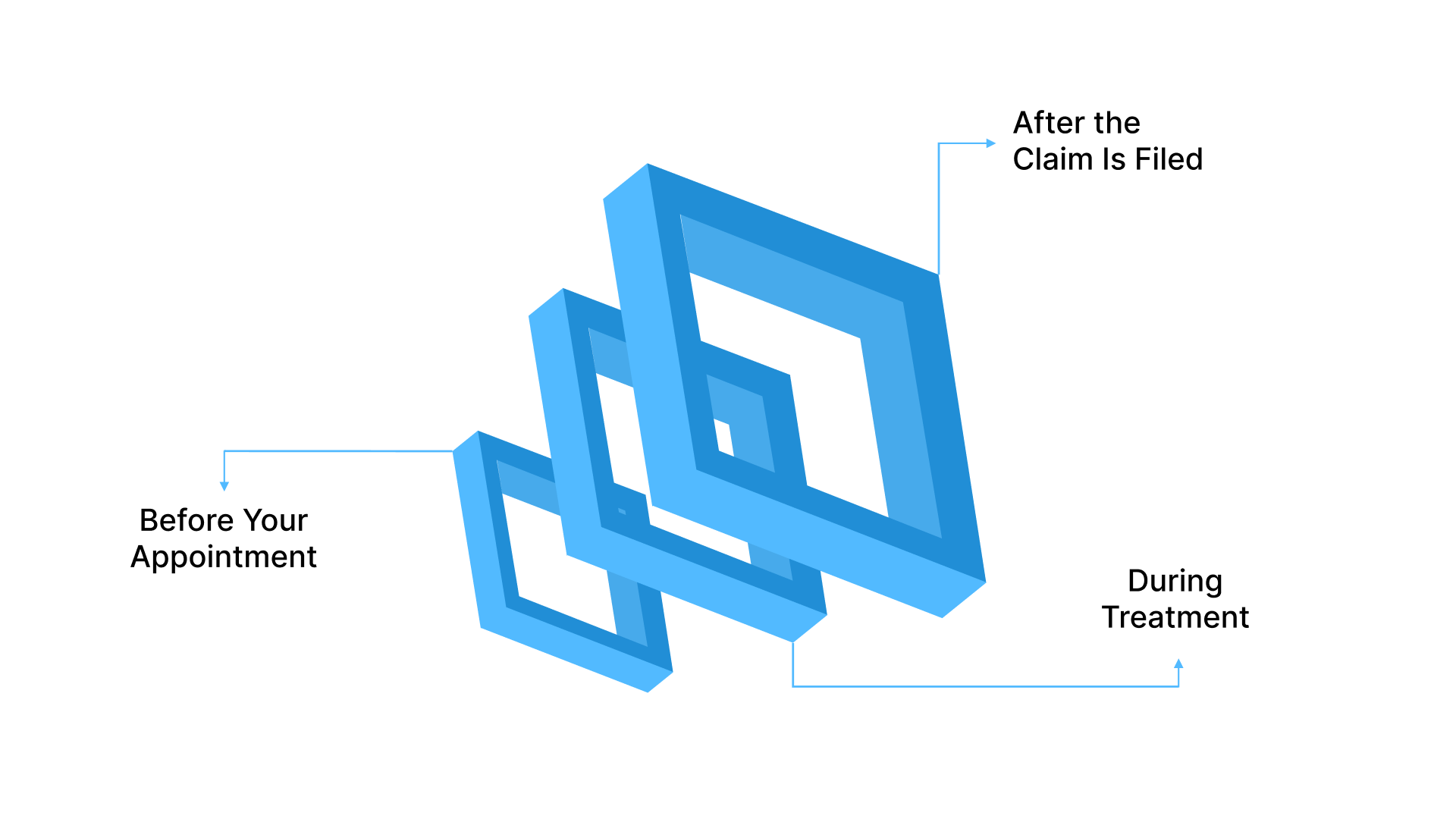
The best way to manage claims is to prevent problems before you even step inside the dental office for care. Being proactive and organized will save you time and money while ensuring that your dental benefits are used efficiently:
Before Your Appointment
Verify that your dentist is currently an active member of your insurance network to ensure you get the lowest rates. You should also request a pre-treatment estimate for any major work to understand your exact out-of-pocket costs in advance.
During Treatment
Ask your dentist to confirm the specific procedure codes they will use for your claim before they begin the work. This conversation ensures that the treatment aligns with your coverage and helps avoid any expensive surprises on your final bill.
After the Claim Is Filed
Review every Explanation of Benefits you receive to ensure the services listed match the work you actually received that day. Keep a digital or physical folder with all your receipts and insurance documents to help you resolve any future disputes.
Following these practices will help you use your dental benefits with complete confidence and avoid any unnecessary financial stress.
The TrueCost Solution for Your Dental Care
Finding dental coverage can feel overwhelming when you are managing a tight monthly household budget. You may feel confused by insurance terms or worry that affordable plans come with hidden limits. Many families stay uninsured because enrollment feels slow, complicated, or unclear.
TrueCost Group removes these barriers by helping you access PPO dental plans with immediate benefits. You receive clear, advisor-guided support through simple messaging so you feel protected before your next dental visit.
Instant Benefit Activation: You can access cleanings and major procedures on day one without waiting for months of prior enrollment.
Direct Messaging Support: You can ask questions and receive plan details through WhatsApp or Messenger for a fast response time.
Transparent Pricing Models: You receive plans with no hidden contracts, which allows you to manage your budget with total financial confidence.
National Network Access: You can choose from over eighty-five thousand dentists to ensure your claims are handled by in-network experts.
Comprehensive Coverage Bundles: You get dental, vision, and hearing benefits in one plan to simplify your family healthcare management tasks.
You can finally stop worrying about the high cost of a healthy smile by choosing a plan designed for life.
Final Thoughts
Managing dental insurance claims does not have to be a confusing or stressful task for you or your family. By understanding the process from treatment to payment, you can ensure your benefits are applied correctly every single time.
This guide has explained how to track claims, read your EOB, and fix common errors to protect your budget. TrueCost Group is here to help you find affordable PPO dental insurance that makes the entire process simple and fast.
We focus on providing plans with immediate benefits so you can get the care you need without any delays. Our team handles the hard work of finding the right plan so you can focus on your dental health.
Get your free quote over text today to see how much you can save on dental care for your family.
FAQs
Q. What Is an Explanation of Benefits (EOB)?
An EOB is a summary sent by your insurer explaining how a claim was processed and what they paid. It shows the dentist's fees, your plan's discounts, and the final amount you may still owe to the dental provider.
Q. Can a Dental Claim Be Refiled?
Yes, your dentist can refile a claim if it was denied due to a simple error or missing clinical information. You should check with the billing department to ensure they have the correct codes before they resubmit the dental paperwork.
Q. Why Did My Dental Claim Get Denied?
Claims are often denied due to plan exclusions, reached annual limits, or simple data entry mistakes on the claim form. Reviewing the denial code on your EOB will tell you the exact reason why the insurer refused to pay.
Q. Can I Appeal a Dental Insurance Claim?
You have the right to appeal a denied claim if you believe the insurance company made an error in judgment. This process usually involves submitting a formal letter and additional dental records to prove that the procedure was medically necessary.
Q. Do Dental Insurance Claims Affect Future Coverage?
Dental insurance claims do not typically cause your monthly premiums to increase as car insurance or home insurance claims would. However, every claim you file counts toward your annual maximum benefit, which resets at the start of each new year.


