
Introduction
Picture this: You've just completed a root canal, feeling relieved that your insurance will cover most of the cost. Two weeks later, a bill arrives for the full $1,200. Your insurance had lapsed three days earlier without your knowledge.
This scenario happens more often than you'd think.
Verifying active dental insurance before treatment is your financial safeguard. According to a 2024 Commonwealth Fund report, 45% of insured adults received a bill for a service they believed was covered. Even more concerning, 17% had recommended services denied coverage despite believing they had active insurance.
Understanding your coverage status before sitting in the dental chair saves you from unexpected bills and financial stress.
This guide walks you through exactly how to verify your dental insurance is active, what information you need, and what to do if coverage has lapsed.
TLDR
- Three verification methods: online portal, phone call to insurer, or dentist's office check
- Have ready: insurance card, policy number, date of birth, and Social Security number
- Verify within 24-48 hours of your appointment, not just when scheduling weeks earlier
- Active policy ≠ covered procedure—verify your plan includes the specific treatment
- Coverage lapsed? Consider COBRA, Medicare Advantage with dental add-ons, or dentist payment plans
What Information You Need to Verify Dental Insurance
Checking your dental insurance status requires specific information from your policy documents and personal records. Having these details ready before you call your insurer or visit your dentist's office will speed up the verification process.
From Your Insurance Card:
- Carrier name (Delta Dental, Aetna, UnitedHealthcare, etc.)
- Policy or group number
- Member ID (unique to you)
- Customer service phone number
- Website URL for online portal access
Personal Verification Information:
- Full legal name (matching your enrollment documents exactly)
- Date of birth
- Social Security number (last 4 digits in most cases)
- If you're a dependent: policyholder's name and relationship
Recent Life Changes That Affect Coverage:
Beyond documentation, consider whether you've experienced recent changes that could affect your coverage status. Certain events can terminate or modify your dental insurance without immediate notification:
- Job loss, reduction to part-time status, or leave of absence
- Marriage, divorce, or legal separation
- Dependent children reaching age 26 (typical coverage cutoff)
- Moving to a new state (may affect network coverage)
- Missed premium payments (can result in retroactive termination)
If any of these apply, documenting the timing and details helps you understand why coverage may have lapsed and what reinstatement options exist.
Methods to Verify Your Dental Insurance Status
Before scheduling dental treatment, confirming your coverage is active can save you from unexpected bills. The verification method you choose depends on how quickly you need answers and how complex your coverage questions are.
Method 1: Online Verification Through Insurance Portal
Most major dental insurers (Delta Dental, Aetna, UnitedHealthcare, Cigna) offer member portals and mobile apps where you can instantly check coverage status, remaining annual maximums, and claim history.
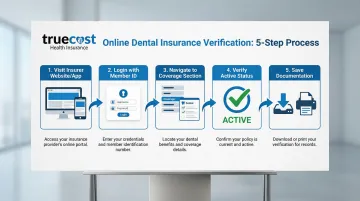
Here's how to verify online:
- Visit your insurer's website or download their mobile app
- Create an account or log in using your member ID and personal information
- Go to "Coverage," "Benefits," or "Eligibility" section
- Verify your policy shows "Active" status with current effective dates
- Screenshot or print the verification page with visible date-stamp for your records
Why this method works:
- Available 24/7 with instant results
- Provides documentation you can save
- Shows additional details like remaining annual maximum and deductible status
Potential drawbacks:
- Portal data may lag 24-48 hours behind recent changes
- Requires prior registration (can't use for urgent same-day verification if not already registered)
- May not reflect retroactive terminations processed after you check
Method 2: Call Insurance Company Directly
If you need the most current information or have specific coverage questions, calling your insurer directly is your best option. A customer service representative can access real-time eligibility data and clarify details about your planned procedures.
When you call:
- Call the customer service number printed on your insurance card
- Provide your member ID, date of birth, and other verification information
- Ask specifically: "Is my dental coverage active as of [your appointment date]?"
- Follow up with: "What services are covered under my plan, and are there waiting periods for [specific procedure]?"
- Document the call: date, time, representative's name, and reference number
Benefits of calling:
- Most reliable for up-to-date information
- Allows clarification of complex coverage questions
- Representative can explain waiting periods, exclusions, and coverage percentages
Keep in mind:
- May involve hold times of 15-20 minutes or longer
- Information is only as accurate as what the representative can access
- No automatic documentation unless you take detailed notes
Method 3: Verify Through Your Dentist's Office
Your dentist's office can handle verification for you as part of their standard workflow. This is the most convenient option, though you'll want to confirm they're checking coverage thoroughly.
- Provide your insurance card to the receptionist when scheduling or checking in
- Ask them to verify both eligibility and coverage details for your planned treatment
- Request a breakdown of estimated out-of-pocket costs based on their verification
- Important: Confirm they verified coverage as of your appointment date, not just when you scheduled weeks earlier
Why patients prefer this:
- Convenient—you're already communicating with the office
- Staff have experience interpreting coverage details and calculating patient responsibility
- Often includes a treatment cost estimate
Possible limitations:
- You're relying on their verification process and accuracy
- Staff may verify coverage weeks before your appointment, missing recent changes
- Staff may verify "eligibility" without confirming specific procedure coverage
Understanding Your Coverage Status and Benefits
Verification reveals more than just "yes" or "no." Understanding the details of your status prevents surprise bills.
Active and Eligible Status
Your policy is current, premiums are paid, and you have access to dental benefits according to your plan's terms. You're in the insurer's system as an active member on the date of service.
What to do next:
- Request a benefits summary showing your deductible status (how much you've paid toward your annual deductible)
- Confirm your annual maximum remaining (only 2.9% of enrollees reach the typical $1,000-$1,500 limit)
- Verify covered services percentages (typically 100% preventive, 80% basic, 50% major)
- Confirm your dentist is in-network if your plan requires it
- Schedule your appointment with confidence
Coverage Active But With Limitations
Even with active coverage, certain services may face restrictions:
- Waiting periods: Common for basic procedures (6-12 months) and major work like crowns or bridges (12 months)
- Annual maximum exhausted: You've used your full benefit for the year
- Specific exclusions: Procedures like implants or cosmetic work may not be covered
- Missing tooth clauses: Some plans won't cover replacing teeth that were missing before your coverage started
Ask your insurer specifically: "Are there waiting periods for [your planned procedure]?" Then review the coverage breakdown:
| Service Category | Typical Coverage | Waiting Period | Examples |
|---|---|---|---|
| Preventive | 100% | None | Cleanings, exams, X-rays |
| Basic | 80% | 6 months | Fillings, extractions |
| Major | 50% | 12 months | Crowns, bridges, dentures |

Next steps:
- Get a detailed cost estimate for your specific procedure
- Consider postponing non-urgent treatment until waiting periods expire
Coverage Lapsed or Terminated
Your policy is no longer active. Common reasons include non-payment of premiums, employment termination, or loss of eligibility. The insurer will not pay claims for services after the termination date.
Critical Issue—Retroactive Termination:
Employers can terminate coverage retroactively. Delta Dental of Arizona allows retroactive termination up to 60 days, while Guardian Life permits up to 90 days for most plans.
You could verify coverage, receive treatment, and then discover weeks later that your coverage was terminated retroactively to a date before your appointment.
If your coverage has lapsed:
- Determine the exact termination date and reason for coverage loss
- Contact your HR department or former employer immediately to investigate
- Explore immediate reinstatement if termination was due to administrative error
- Investigate COBRA continuation coverage if you lost employer-sponsored insurance (see section below)
- Research alternative coverage options before proceeding with treatment
- If you've received treatment, document your verification attempts to demonstrate due diligence
Common Mistakes When Verifying Dental Insurance
Not Verifying Coverage Close to Date of Service
Eligibility can change retroactively due to employer reporting delays. Verification done weeks in advance may be outdated by your appointment date.
To protect yourself from unexpected bills, verify your eligibility on the date of service according to American Dental Association guidelines. At minimum, re-verify within 24-48 hours of your appointment—especially for procedures costing over $500.
Confusing Eligibility with Benefits Coverage
A representative saying "yes, you're eligible" confirms you're in the system. It doesn't guarantee your specific treatment is covered or that you've met requirements like waiting periods.
Ask these two distinct questions every time:
- "Is my coverage active on [appointment date]?"
- "Is [specific procedure] a covered service under my plan, and are there any waiting periods or exclusions?"
These questions clarify both your enrollment status and your actual benefits.
Failing to Verify After Life Changes
Trigger events often affect dental coverage immediately, but notification delays mean you may not realize coverage has ended.
Common Trigger Events:
- Job loss or reduction to part-time status
- Leave of absence (FMLA, personal, medical)
- Divorce or legal separation
- Dependent child turning 26
- Moving to a new state
Verify coverage immediately after any of these events. Don't wait for official termination notices—they often arrive after coverage has already ended.
Not Documenting Verification Attempts
If your insurer later denies a claim, you'll need proof of your verification attempts. Without documentation, you have no evidence of what information representatives provided.
Build a verification file containing:
- Screenshots of portal verifications (with visible date-stamps)
- Written notes from phone calls (date, time, representative name, reference number)
- Copies of benefits summaries
- Photos of both sides of your insurance card
While documentation doesn't guarantee you won't be held liable for bills, it provides evidence of due diligence if disputes arise.

What to Do If Your Coverage Is Inactive or Insufficient
Discovering you lack dental coverage when you need treatment is stressful, but several options can help you manage the situation.
Immediate Steps If Coverage Has Lapsed
- Contact your HR department or former employer immediately to understand why coverage ended
- Ask about retroactive reinstatement if termination was due to administrative error
- Request documentation of your coverage termination date in writing
- Don't proceed with treatment until you've resolved the coverage question or arranged alternative payment
COBRA Continuation Coverage
If you lost employer-sponsored dental insurance due to job loss or other qualifying events, COBRA allows you to continue coverage for specific periods.
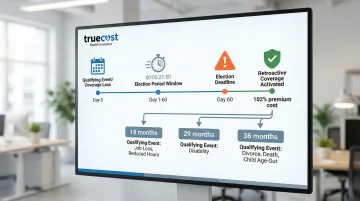
Key COBRA Details:
- You pay the full group premium plus a 2% administrative fee (102% total)
- You have 60 days from the qualifying event to elect COBRA
- COBRA provides retroactive coverage to your termination date if you elect within the window
- This prevents gaps and covers services received during the election period
- Coverage duration: 18 months standard (29 months for disability, 36 months for divorce or dependent aging out)
Exploring Alternative Coverage Options
If COBRA isn't viable, consider these coverage alternatives:
Individual Dental Insurance Plans:
- Research standalone plans through private insurers in your state
- Expect waiting periods of 6-12 months for major procedures
- May delay coverage for immediate treatment needs
Comprehensive Health Plans with Dental Benefits:
Some health insurance options include dental coverage:
ACA Marketplace Plans: Dental coverage is required for children under 18 but optional for adults. Stand-alone dental plans (SADPs) are available in every state, though they generally don't qualify for premium subsidies.
Medicare Advantage Plans: Original Medicare doesn't cover routine dental care, but many Medicare Advantage plans include dental as a supplemental benefit. Many plans include dental, vision, and hearing coverage as additional benefits beyond standard Medicare. If you're Medicare-eligible, these comprehensive plans may provide better value than standalone dental insurance.
Dental Discount Plans:
For immediate needs without traditional insurance, dental discount plans offer an alternative. These aren't insurance—they're fee-reduction programs where you pay discounted rates directly to participating dentists. There are no claims, no annual maximums, and no waiting periods, making them useful for immediate treatment needs.
Discuss Payment Alternatives With Your Dentist
Even without insurance, you have options. Many dental offices offer flexible payment arrangements:
- In-house payment plans: Monthly installments with little or no interest
- Healthcare financing: CareCredit or similar medical credit cards
- Cash discounts: Some practices offer 5-10% discounts for upfront payment
- Adjusted treatment plans: Prioritizing urgent care and phasing non-urgent procedures over time
Best Practices for Maintaining Active Dental Coverage
Establish a Verification Routine
Before Major Dental Work:
- Verify coverage when scheduling the appointment
- Re-verify within 24-48 hours of your appointment date
- Confirm specific procedure coverage, not just eligibility
General Coverage Checks:
- Do a complete coverage review every 6 months
- Verify after any employment or life status change
- Check remaining annual maximum benefits before year-end
Document Everything
Keeping detailed records protects you if coverage questions arise later.
Create a coverage file (digital or physical) containing:
- Portal screenshots showing date, time, and "Active" status
- Phone call logs with representative names, reference numbers, and timestamps
- Current benefits summary (deductible status, annual maximum, coverage percentages)
- Photos of both sides of your insurance card
Monitor for Life and Employment Changes
Major life events can affect your coverage status without warning.
Set calendar reminders to verify coverage immediately after:
- Changing jobs, losing employment, or moving to part-time status
- Getting married, divorced, or legally separated
- Moving to a new state or coverage area
- Children aging out at 26 or dependents losing eligibility
- Receiving any employer notice about plan modifications
Frequently Asked Questions
How long does it take to verify dental insurance?
Online portals take 2-5 minutes once registered, while phone verification takes 10-20 minutes including hold time. Your dentist's office can verify during check-in, though detailed benefit breakdowns may take 24 hours.
Can I verify my dental insurance online without calling?
Most major dental insurers offer online portals and mobile apps for instant verification after you register with your member ID. Phone verification is still recommended before major procedures to confirm current coverage details.
What information do I need to verify my dental insurance?
You'll need your insurance card with policy and member ID numbers, your date of birth, Social Security number, and if you're a dependent, the policyholder's information. Have your insurance card ready before calling or logging into the portal.
What if my dentist says I have coverage but my insurance says I don't?
Request documentation from both parties showing what they verified and when. Contact your insurance company directly to understand the discrepancy. Do not proceed with treatment until the coverage question is fully resolved—you could be held financially responsible if coverage disputes remain unresolved.
Do I need to verify my dental insurance before every appointment?
Verify before major procedures or if it's been more than 6 months since your last appointment. Routine cleanings with established, stable coverage need less frequent verification. Always verify immediately after any employment or life changes that could affect eligibility.
What happens if I get treatment and my insurance was actually inactive?
You become personally responsible for the full treatment cost, and the dentist may pursue collection. Even with documentation proving you verified coverage, retroactive coverage changes often leave patients liable for bills.
Protecting yourself from surprise dental bills starts with thorough verification. Take the time to confirm your coverage is active, understand what procedures are covered, and document your verification attempts.
If navigating dental insurance feels overwhelming or you're currently uninsured, comprehensive health plans through the ACA marketplace or Medicare Advantage often include dental, vision, and hearing benefits. TrueCost Group's licensed advisors can help you explore plans starting at $0-$50/month for qualified individuals. Call 1-888-788-8285 to find coverage that meets your healthcare needs.


