Introduction
Approximately 10 million wisdom teeth are removed from roughly 5 million Americans each year, making it one of the most common oral surgery procedures. If you're facing wisdom teeth extraction, you're probably wondering: How bad will the pain be? How long until I can eat normally? What if something goes wrong?
The good news: recovery follows a predictable pattern, with most discomfort concentrated in the first 3-5 days. Understanding what to expect at each stage helps you distinguish between normal healing and warning signs that require immediate attention.
You'll learn the complete recovery timeline, essential care instructions, and red flags that should prompt a call to your oral surgeon. We'll also cover how insurance typically handles this common procedure—important information if you're concerned about out-of-pocket costs.
TLDR: Quick Recovery Overview
- Full recovery takes 1-2 weeks, with the most discomfort during days 1-5
- Swelling peaks around day 2-3, while pain typically intensifies around day 3-4 before improving
- Following post-op instructions prevents dry socket (affects 3-4% of extractions)
- Call your surgeon immediately for bleeding beyond 4 hours, fever >101°F, worsening pain after day 4, or pus
- Most ACA and Medicare Advantage plans cover medically necessary wisdom teeth removal with proper documentation
Immediate Aftermath: The First 24-48 Hours
What to Expect Leaving the Office
You'll leave the dental office with gauze packed over the extraction sites, feeling numbness from local anesthesia that typically lasts 2-4 hours.
If you received sedation or general anesthesia, grogginess may persist for several hours. You'll need someone to drive you home and stay with you initially.
Managing Bleeding
Expect oozing blood for 24-48 hours after surgery. Here's how to manage it:
- Bite firmly on gauze for 30 minutes after surgery
- Bleeding generally slows within 3-4 hours, though minor spotting may continue
- Replace gauze as needed, maintaining firm pressure
- Watch for bright red spurts or bleeding that doesn't slow after 4 hours of pressure
Pain and Swelling Control
Discomfort is normal. Swelling peaks around days 2-3 and gradually subsides over the following week.
Ice pack schedule for the first 24-48 hours:
- Apply for 20 minutes, then remove for 20 minutes
- Continue this cycle while awake during the first two days
- Ice helps minimize initial inflammation and provides numbing relief
Pain medication:
- Take prescribed or recommended pain medication before numbness wears off
- Follow the dosing schedule consistently for the first 48 hours
- Don't wait until pain becomes severe to take medication
First 48 Hours: Dietary Guidelines
Your diet directly impacts healing during this critical window. Stick exclusively to soft, cool, or room-temperature foods:
- Yogurt, applesauce, smoothies (eaten with a spoon), pudding, lukewarm soup, mashed potatoes
- Avoid hot foods while numb to prevent accidental burns and increased bleeding
- Nothing that requires chewing or could irritate extraction sites
Critical Activities to Avoid
Avoid straws for at least 3-5 days. The suction action can dislodge the blood clot protecting your extraction site, leading to painful dry socket.
Do not smoke. Smoking impairs healing and increases dry socket risk more than threefold compared to non-smokers.
Don't rinse your mouth on the day of surgery. Aggressive swishing can dislodge protective blood clots.
Avoid strenuous activity. Physical exertion increases blood pressure, which can trigger bleeding and swelling.
Sleep with your head propped on 2-3 pillows for the first 48 hours to minimize swelling and bleeding.

Week 1 Recovery: Daily Progression and What to Expect
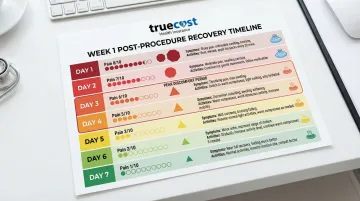
Day-by-Day Symptom Timeline
Days 1-2: The immediate post-surgery phase
- Peak bleeding and numbness wearing off
- Pain increases as anesthesia fades
- Begin taking pain medication on schedule
- Maintain ice pack routine
Days 3-4: The hardest stretch
- Swelling reaches its maximum
- Pain often peaks during this window
- This is typically the most uncomfortable phase
- Improvement should begin after day 4
By day 5-7: Turning the corner
- Noticeable reduction in swelling
- Pain becomes more manageable
- You'll feel more energetic
- Dietary options gradually expand
Transitioning to Warm Compresses
As you hit the peak swelling phase around days 3-4, you can transition from ice to warm compresses. Gentle heat helps improve circulation and promotes healing, but timing matters—applying heat too early may actually increase swelling.
Saltwater Rinse Protocol
Begin gentle saltwater rinses the day after surgery (not on surgery day). Dissolve 1/2 teaspoon of salt in a cup of warm water.
Proper technique:
- Gently soak the area rather than vigorously swishing
- Rinse 3-4 times daily, especially after meals
- Avoid forceful swishing that could dislodge blood clots
Gradual Diet Progression
First 3 days: Liquids and very soft foods only (yogurt, applesauce, smoothies)
Middle of the week: Introduce semi-soft foods as comfort allows:
- Scrambled eggs
- Well-cooked pasta
- Mashed potatoes
- Soft bread (torn into small pieces)
- Oatmeal or cream of wheat
Avoid crunchy, hard, or chewy foods like popcorn, nuts, chips, and tough meats for at least 2 weeks—these could irritate healing sites.
Oral Hygiene During Week 1
- Resume gentle brushing after 24 hours, carefully avoiding extraction sites
- Don't brush directly on or near the surgical areas for the first week
- Gently brush your tongue to prevent bad breath from healing tissue
- Use minimal toothpaste and rinse very gently
Week 2 and Beyond: The Healing Timeline
Complete Healing Stages
Your extraction sites heal in stages:
- Stitches (if applicable): Dissolvable sutures usually disappear within 1-2 weeks. Small threads coming loose is normal.
- Soft tissue closure: Gum tissue begins closing around the extraction site between days 6-14.
- Bone healing: Bone healing starts after one week, with substantial filling by 10 weeks. Full bone remodeling continues for 3-6 months beneath the surface, but won't affect your daily activities.

Returning to Normal Activities
Diet: Most patients can return to a normal diet by week 2, though you may want to avoid extremely crunchy or hard foods for a bit longer.
Exercise: Most patients can resume fitness routines within 48-72 hours for simple extractions. Wait for your surgeon's approval before resuming strenuous activity, especially if you had complex surgical extractions.
Work/School: Typical recovery time is 2-3 days for simple extractions and 5-7 days for complex cases, depending on your job requirements and the type of anesthesia used.
Long-Term Considerations
- Jaw stiffness: Temporary jaw tightness is common and usually resolves within 7-10 days with gentle jaw exercises
- Bite changes: Slight changes in how your teeth come together may occur but usually resolve as swelling completely subsides
- Follow-up: Schedule any recommended follow-up appointments, usually 1-2 weeks after your procedure
Essential Do's and Don'ts During Recovery
Do's
- Rest with elevation: Keep your head elevated, especially during the first 48 hours
- Medication schedule: Take prescribed medications exactly as directed, on time
- Stay hydrated: Drink plenty of water (no straws) to support healing
- Soft food diet: Follow dietary restrictions carefully to protect extraction sites
- Gentle oral hygiene: Resume careful brushing and saltwater rinses after 24 hours
Don'ts
- No straws: Suction creates negative pressure that can dislodge blood clots, causing dry socket
- No smoking or vaping: Smokers face a 13.2% dry socket rate versus 3.8% for non-smokers
- **Avoid alcohol: It interferes with healing and interacts with pain medications
- Don't touch extraction sites: Avoid poking with your tongue or fingers, which brings in bacteria
- No vigorous rinsing: Gentle soaking only—aggressive swishing disrupts healing
Additional Care Tips
Work and school planning: Most people need 2-3 days off for simple extractions.
If your job involves physical labor, speaking extensively, or high stress, plan for 5-7 days of recovery time.
Sleep positioning: Sleep on your back with your head elevated on 2-3 pillows for the first week.
If you must sleep on your side, avoid the extraction side.
Normal healing signs:
- Slight yellow or white film over extraction sites (healing tissue, not infection)
- Gradual reduction in swelling after day 3-4
- Pain that steadily improves after day 4-5
- Minor oozing that decreases daily

Warning Signs: When to Call Your Dentist Immediately
Emergency Symptoms Requiring Same-Day Contact
Contact your oral surgeon immediately if you experience:
- Excessive bleeding: Bright red blood that doesn't stop after 4 hours of consistent gauze pressure
- High fever: Temperature above 101°F (38.3°C) indicating possible infection
- Severe uncontrolled pain: Pain that doesn't respond to prescribed medication or worsens significantly after day 4
- Difficulty breathing or swallowing: May indicate serious swelling or allergic reaction
One of the most common post-extraction complications requires detailed attention: dry socket.
Dry Socket: A Detailed Explanation
What it is: Dry socket (alveolar osteitis) happens when the protective blood clot at your extraction site dislodges or dissolves too early, exposing bone underneath.
Incidence rates: Dry socket affects 1-5% of routine extractions but can reach 30% for surgically impacted wisdom teeth.
Symptoms:
- Severe, throbbing pain starting 1-5 days post-surgery (typically around day 3-5)
- Pain radiating to your ear, eye, temple, or neck
- Visible bone in the extraction socket
- Bad breath and foul taste that won't go away
- Partial or complete loss of the blood clot
Why immediate treatment matters: Dry socket requires professional treatment with medicated dressings to relieve pain and promote healing. It won't resolve on its own.
Signs of Infection
Watch for these infection indicators:
- Persistent or worsening swelling after day 3-4 (swelling should decrease, not increase)
- Pus discharge from extraction sites—yellow, green, or white drainage
- Increasing pain rather than gradual improvement after day 4
- Fever above 101°F accompanied by chills or feeling generally unwell
- Difficulty swallowing or breathing indicating possible abscess formation
Nerve Damage Symptoms
While infections and dry socket are more common, another rare but serious complication to monitor is nerve injury:
Incidence: Temporary nerve injury affects 1-3% of extractions, with permanent injury occurring in less than 2% of cases.
Symptoms to watch for:
- Numbness, tingling, or altered sensation in your tongue, lips, or chin
- Symptoms persisting beyond the expected anesthesia timeframe (4-8 hours)
- Changes in taste perception
- Difficulty with speech or tongue movement
If you experience any of these symptoms beyond the first day, contact your oral surgeon for evaluation. Most post-operative complications require professional treatment, and if you have health insurance coverage, these follow-up visits are typically covered under your plan's surgical benefits.
Understanding the Cost and Insurance Coverage
National Cost Ranges
Wisdom teeth removal costs vary significantly based on complexity and geographic location. Expect to pay within these ranges:
- Simple extraction: $200-$1,100 per tooth
- Impacted extraction: $225-$600+ per tooth
- Fully bony impaction: $319-$707 per tooth depending on complexity
Factors Affecting Pricing
Several factors influence your final bill:
- Costs increase with impaction depth—erupted teeth cost less than partially or fully impacted teeth requiring surgical extraction
- Local anesthesia is typically included, while IV sedation or general anesthesia adds $200-$600
- Urban areas and high cost-of-living regions have higher dental surgery fees
- Removing all four wisdom teeth at once may offer package pricing that reduces the per-tooth cost
Insurance Coverage Options
Dental insurance typically covers 50-80% of wisdom teeth removal costs, with the percentage depending on whether the procedure is classified as basic or major.
Medical insurance may cover the procedure when deemed medically necessary—such as for infection, cysts, tumors, damage to adjacent teeth, or non-restorable cavities.
Finding Affordable Health Coverage
If you lack health insurance, comprehensive plans through the ACA marketplace may include coverage for medically necessary oral surgery. TrueCost Group helps Americans find affordable health insurance through the ACA marketplace and Medicare Advantage plans, with 80% of clients qualifying for plans starting at $0-$50 per month.
Their licensed advisors can help you understand whether available health plans include coverage for medically necessary procedures like wisdom teeth removal.
To explore health insurance options that may cover oral surgery, contact TrueCost Group at 1-888-788-8285 or visit their website to learn about plans from major carriers like UnitedHealthcare, Aetna, and BlueCross BlueShield.
Frequently Asked Questions
How long does pain last after wisdom teeth removal?
Most pain subsides within 3-5 days, typically peaking around day 3-4 before gradually improving. Pain should be manageable with prescribed or over-the-counter medication and should steadily decrease after day 5.
Can I go to work or school the day after wisdom teeth removal?
Most people need 2-3 days off for simple extractions and 5-7 days for complex cases, depending on job requirements and anesthesia type.
What are the signs of dry socket and how common is it?
Dry socket causes severe pain around day 3-5, bad breath, foul taste, and visible bone in the socket. It occurs in 1-4% of routine extractions, with significantly higher rates (up to 30%) for impacted teeth. Smokers face three times the risk of non-smokers.
When can I eat solid foods after wisdom teeth removal?
Progress gradually: liquids and soft foods for days 1-3, semi-soft foods like eggs and pasta for days 4-7, then return to normal diet around week 2.
Is it normal to have bad breath after wisdom teeth removal?
Yes, temporary bad breath is common due to food particles trapped in healing sites, limited brushing, and healing tissue. Gentle saltwater rinses after 24 hours and careful oral hygiene help minimize odor. Bad breath should improve within 7-10 days.
Does health insurance cover wisdom teeth removal?
Dental insurance typically covers 50-80%, while medical insurance may cover medically necessary procedures. Licensed advisors at TrueCost Group can help you explore health insurance plans that may include oral surgery benefits—call 1-888-788-8285.